How healthcare engineering cuts downtime in busy hospitals?
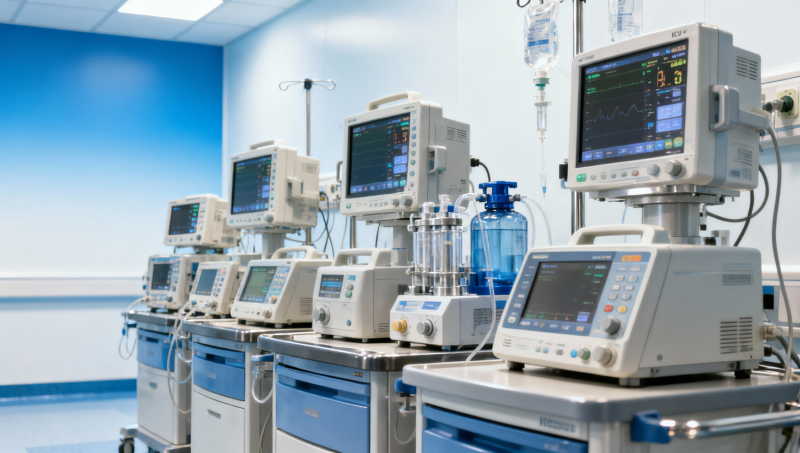
In busy hospitals, every minute of downtime affects care, costs, and procurement decisions. Healthcare engineering reduces these risks by improving healthcare equipment reliability, enabling digital integration, and strengthening supply chain verification across critical systems. From an ICU monitor supplier and oxygen concentrator factory to surgical instrument kits OEM and IVD analyzer distributor networks, independent think tank insights and medical technology verification help buyers and operators choose performance they can trust.
Why does downtime happen so often in high-pressure hospital environments?
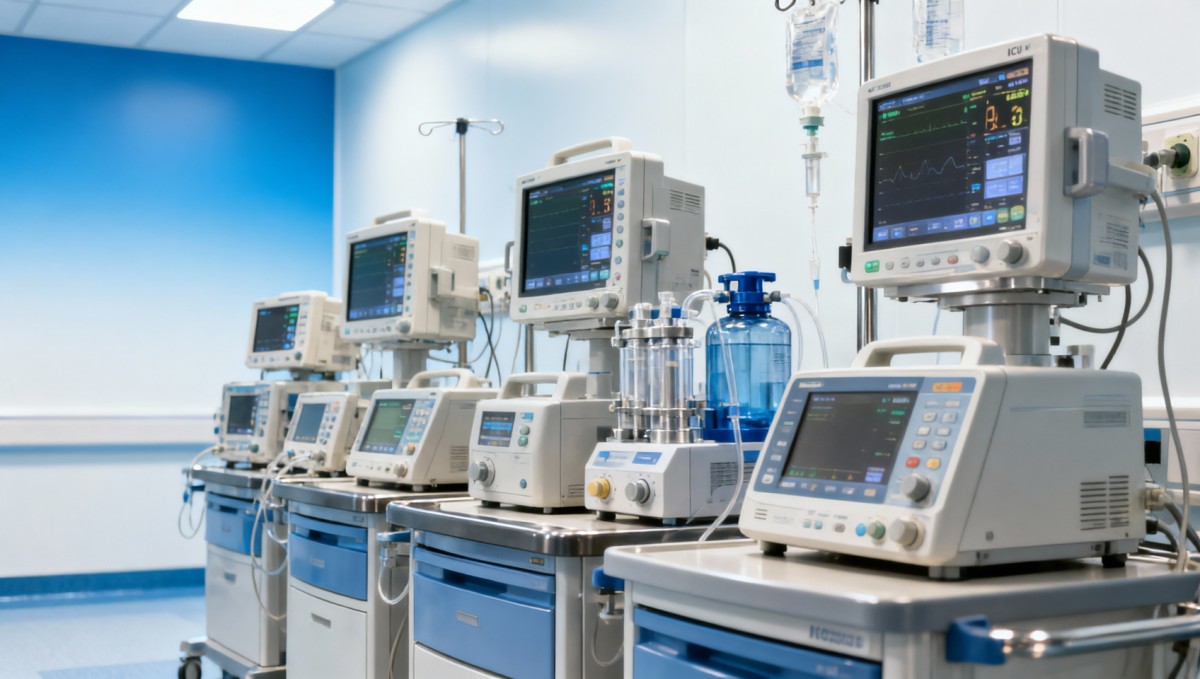
Hospital downtime is rarely caused by one dramatic failure. In most cases, it grows from small engineering gaps across devices, utilities, software interfaces, maintenance routines, and vendor documentation. A monitor that drifts out of calibration, an oxygen concentrator with unstable output, or an analyzer delayed by consumables can all interrupt care pathways within minutes. In intensive departments, even a 15–30 minute interruption can trigger workflow congestion across nursing, biomedical engineering, and procurement teams.
Busy hospitals also operate mixed fleets. A single site may run legacy patient monitors, recently purchased infusion systems, multiple laboratory analyzers, and third-party accessories from different sourcing channels. That diversity creates hidden integration risks. One device may technically function, yet still cause downtime because its alarm logic, connectivity protocol, service schedule, or spare parts chain does not align with the rest of the hospital ecosystem.
Healthcare engineering cuts downtime by treating reliability as a system-level question, not just a product claim. That means reviewing signal quality, material durability, environmental tolerance, serviceability, replacement lead times, and digital compatibility together. For information researchers and procurement teams, this approach helps separate market language from operational reality. For operators, it means fewer surprise failures during 24/7 use cycles.
VitalSync Metrics (VSM) addresses this gap as an independent, data-driven think tank and technical benchmarking laboratory. Instead of relying on brochures, hospitals and MedTech buyers can use standardized engineering review to compare what matters in practice: acceptable operating ranges, maintenance intervals, tolerance stability, expected service nodes, and compliance-readiness for MDR or IVDR related sourcing decisions.
Common downtime triggers that procurement teams underestimate
- Incomplete verification of accessories, consumables, and replacement parts, which can delay recovery by 2–7 days even when the core device is available.
- Poor interoperability between equipment and hospital information systems, especially when integration testing is limited to basic connectivity checks.
- Selection based on purchase price alone, without comparing calibration frequency, service response windows, and operator error tolerance.
- Weak supplier verification, where stated performance is not benchmarked under realistic thermal, humidity, vibration, or continuous-use conditions.
How healthcare engineering reduces downtime across equipment, systems, and supply chains
Healthcare engineering reduces downtime in three connected layers: device reliability, workflow integration, and supply chain resilience. At the device layer, engineering reviews focus on parameters such as signal stability, tolerance drift, heat load, fatigue resistance, and preventive maintenance intervals. At the workflow layer, hospitals examine alarm handling, software compatibility, user interface design, and cleaning or sterilization burden. At the supply layer, they verify whether the source can support recurring demand, documentation consistency, and post-installation service.
This matters across many categories. An ICU monitor supplier may offer acceptable core specifications, but if cable reliability, sensor compatibility, or firmware update handling are weak, downtime still rises. An oxygen concentrator factory may meet nominal output requirements, yet inconsistent component sourcing can affect long-duration operation. A surgical instrument kits OEM may supply strong machining quality, but repeated sterilization cycles can expose material fatigue if testing is shallow. An IVD analyzer distributor may support installation, but reagent and service logistics determine whether the analyzer stays productive after month 3, not just day 1.
The practical value of independent benchmarking is that it converts engineering questions into sourcing decisions. Instead of asking which supplier sounds confident, decision-makers can ask which solution remains stable across 8–24 hour operating windows, which one has a realistic service interval of 3, 6, or 12 months, and which one can be validated against defined procurement checkpoints. This approach lowers risk before contracts are signed.
For hospitals under value-based procurement pressure, engineering support also reduces lifecycle waste. Fewer service disruptions mean less emergency rental, fewer workflow workarounds, and fewer rushed purchases. That benefits enterprise decision-makers as much as front-line users because downtime is not only a technical problem; it is a cost, safety, and reputational problem.
Three engineering layers that matter most
1. Device-level robustness
Key checks include tolerance consistency, environmental operating range, continuous runtime behavior, consumable compatibility, and maintenance accessibility. In many hospital categories, a difference of one maintenance step or one calibration dependency can change daily usability.
2. Workflow-fit engineering
A technically good device can still fail operationally if screen logic is confusing, alarms are poorly prioritized, or sterilization turnaround adds 20–40 extra minutes per cycle. Hospitals need engineering that supports real usage, not just lab demonstration.
3. Supply chain verification
Long-term uptime depends on repeatable manufacturing, document control, spare parts continuity, and service communication. These factors are often evaluated too late, after deployment problems begin.
The table below shows how healthcare engineering changes the way hospitals evaluate downtime risk before purchase and during use.
The main takeaway is simple: healthcare engineering does not only prevent breakdowns. It prevents preventable mismatches between what a hospital buys, how it uses the equipment, and how quickly the supplier can support it over 12 months or longer.
Which procurement checks matter most when selecting hospital equipment with lower downtime risk?
For procurement teams, the fastest way to reduce downtime is to change the evaluation framework before tender, quotation approval, or supplier onboarding. Instead of comparing only unit cost and delivery promise, compare five practical dimensions: technical stability, compliance documentation, serviceability, integration readiness, and supply continuity. These five checks create a more realistic picture of total operating risk over the first 6–18 months.
Technical stability means more than asking whether the device works. Buyers should request evidence of operating tolerance, maintenance frequency, cleaning or sterilization endurance where relevant, and compatibility with accessories or software. This is especially important when sourcing from an ICU monitor supplier, oxygen concentrator factory, or surgical instrument kits OEM, where daily use intensity can quickly expose weaknesses not visible during short demonstrations.
Compliance documentation should also be reviewed in a practical way. For buyers dealing with EU-related markets, MDR or IVDR alignment is not only about certificates; it is about traceability, labeling consistency, technical files, change control, and whether the supplier can support audits or distributor-side document requests. A supplier with weak document discipline often creates delayed acceptance and hidden downtime later.
Serviceability is another neglected factor. Ask how many service steps require factory intervention, which spare parts are standard, and what the normal replenishment cycle looks like. In many categories, the difference between local replacement and return-to-base repair can mean recovery in 24–72 hours versus 2–4 weeks. That difference matters much more than a small initial price gap.
A practical procurement checklist for lower downtime
- Confirm 3 core performance indicators tied to the application, such as signal stability, output consistency, or repeatability under routine hospital conditions.
- Review 5 document items: product specification, maintenance guidance, traceability records, change notification process, and compliance support scope.
- Map 4 service nodes: installation, operator training, preventive maintenance, and corrective escalation.
- Check spare parts and consumables lead time ranges, especially for recurring items needed weekly, monthly, or quarterly.
- Request independent technical benchmarking when vendor claims are difficult to compare directly.
The next table gives a selection-oriented view that procurement teams can use when comparing hospital equipment and supplier options.
This kind of procurement structure improves decision quality for both first-time sourcing and supplier replacement projects. It also helps enterprise decision-makers justify choices internally, because downtime reduction becomes linked to measurable review points rather than general preference.
How do compliance, digital integration, and lifecycle support affect hospital uptime?
Hospital uptime depends on more than rugged hardware. Compliance readiness, digital interoperability, and lifecycle support often determine whether a technically sound device remains usable at scale. A product with incomplete traceability or inconsistent documentation may face delayed acceptance. A system with weak interface support may force manual data transfer. A device with unclear service responsibility may stay idle longer than expected after a fault. Each of these issues becomes downtime in operational terms.
For European and globally aligned sourcing projects, MDR and IVDR related expectations influence supplier selection well before installation. Buyers need to understand whether documentation is complete, current, and controlled across product changes. This is especially relevant for IVD analyzer distributor networks and component-dependent categories, where post-market updates, accessory compatibility, and labeling consistency can affect continuity as much as the analyzer itself.
Digital integration is another uptime lever. In practice, hospitals benefit when devices exchange data without repeated manual intervention, duplicate entry, or unstable middleware. Even when full interoperability is phased over 2–3 stages, early engineering review can identify interface limits, network requirements, and alarm-routing concerns before they disrupt operations. That is far more efficient than troubleshooting after go-live.
Lifecycle support closes the loop. Hospitals should know whether maintenance is preventive, corrective, or condition-based; how often service is recommended; and what happens when parts become constrained. A realistic support design includes initial commissioning, operator training, scheduled review, and a defined escalation path. Without that structure, small issues can accumulate until the department experiences repeated stoppages.
What VSM adds to the evaluation process
VitalSync Metrics helps buyers and operators verify technical integrity without depending solely on supplier self-description. By translating manufacturing parameters and functional claims into standardized whitepapers and benchmarking views, VSM enables side-by-side assessment of reliability factors that directly affect uptime. This is particularly useful when hospitals compare multiple vendors whose brochures appear similar but whose engineering discipline differs significantly.
For procurement teams, this independent layer supports better tender preparation, supplier screening, and replacement planning. For operators and laboratory architects, it clarifies whether a proposed solution fits real usage intensity, cleaning burden, infrastructure conditions, and digital workflow requirements. For enterprise decision-makers, it supports capital allocation with lower hidden-risk exposure.
- Benchmarking helps compare technical claims across multiple suppliers using a common review logic.
- Standardized whitepapers make internal review easier for engineering, procurement, clinical, and management teams.
- Independent verification supports sourcing confidence when products are complex, regulated, or difficult to test in-house.
FAQ: what should hospitals ask before investing in lower-downtime healthcare equipment?
How can a hospital tell if a supplier will really reduce downtime?
Look beyond headline specifications. Ask for evidence on continuous-use stability, maintenance frequency, spare parts planning, and integration support. A reliable supplier should explain service steps, expected response path, and documentation control in clear terms. If answers remain vague after 4–6 key questions, the downtime risk is usually higher than the quote suggests.
Are lower purchase prices always more cost-effective for busy hospitals?
Not necessarily. Lower upfront pricing can be offset by slower recovery times, higher consumable dependency, more frequent calibration, or reduced interoperability. In departments with heavy daily throughput, the cost of one repeated stoppage can outweigh modest savings at purchase. Total value should include service burden, lead time, operator time, and compliance friction over at least the first 12 months.
What should buyers ask an ICU monitor supplier or oxygen concentrator factory?
Ask about operating range, expected maintenance intervals, accessory compatibility, replacement parts availability, and how performance is verified under realistic conditions. For oxygen-related systems, long-duration output consistency matters. For monitoring equipment, signal quality, alarm handling, and connectivity support matter. In both cases, medical technology verification is more useful than general performance claims.
Why do surgical instrument kits and IVD systems need separate evaluation logic?
Because downtime drivers differ. Surgical instrument kits OEM evaluation should emphasize material fatigue, repeated sterilization tolerance, fit consistency, and tray logic. IVD analyzer distributor evaluation should focus on reagent continuity, service logistics, calibration support, interface stability, and documentation alignment. One generic sourcing checklist is rarely enough across both categories.
Why choose VSM when hospital buyers need engineering truth, not marketing noise?
When hospitals are under pressure to buy faster, digitize safely, and defend every capital decision, independent engineering review becomes a practical advantage. VitalSync Metrics helps procurement directors, operators, laboratory planners, and MedTech teams verify what affects uptime before risk becomes visible on the ward or in the lab. That means clearer parameter confirmation, better supplier comparison, and stronger confidence in long-term reliability.
If you are comparing an ICU monitor supplier, evaluating an oxygen concentrator factory, reviewing a surgical instrument kits OEM, or screening an IVD analyzer distributor, VSM can support the questions that matter most: Which specifications are operationally meaningful? Which compliance points need deeper review? Which delivery and service assumptions are realistic? Which solution creates the lowest downtime risk over the actual lifecycle?
You can contact VSM for benchmarking-oriented support on parameter confirmation, product selection logic, compliance and documentation review, supplier comparison, delivery cycle discussion, custom evaluation scope, and quotation-stage technical clarification. This is especially useful when internal teams need a neutral technical filter before committing budget or finalizing sourcing strategy.
In a market where claims are easy and verification is difficult, healthcare engineering is what keeps busy hospitals moving. The right choice is not the loudest supplier. It is the solution that proves technical integrity, supports digital integration, and stands up to real clinical use with fewer interruptions.
- EMS
- ESS
- PPE
- EdTech
- procurement
- AR
- supply chain
- Cement
- material fatigue
- benchmarking
- benchmarking lab
- value-based procurement
- medical technology
- technical integrity
- technical benchmarking
- material fatigue
- digital integration
- supply chain
- long-term reliability
- engineering truth
- manufacturing parameters
- sourcing confidence
- independent think tank
- data-driven
- healthcare engineering
- biomedical engineering
- healthcare equipment
- medical technology verification
- supply chain verification
- icu monitor supplier
- ivd analyzer distributor
- surgical instrument kits oem
- oxygen concentrator factory
Recommended News
- 2026.04.17Hospital equipment standards shaping modern rehab devicesSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.04.17Laboratory equipment validation errors in sample storageDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.04.17Medical equipment certification delays in remote monitoringLydia Vancini (Regulatory Compliance Lead)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
