When remote monitoring data triggers unexpected FDA reporting obligations
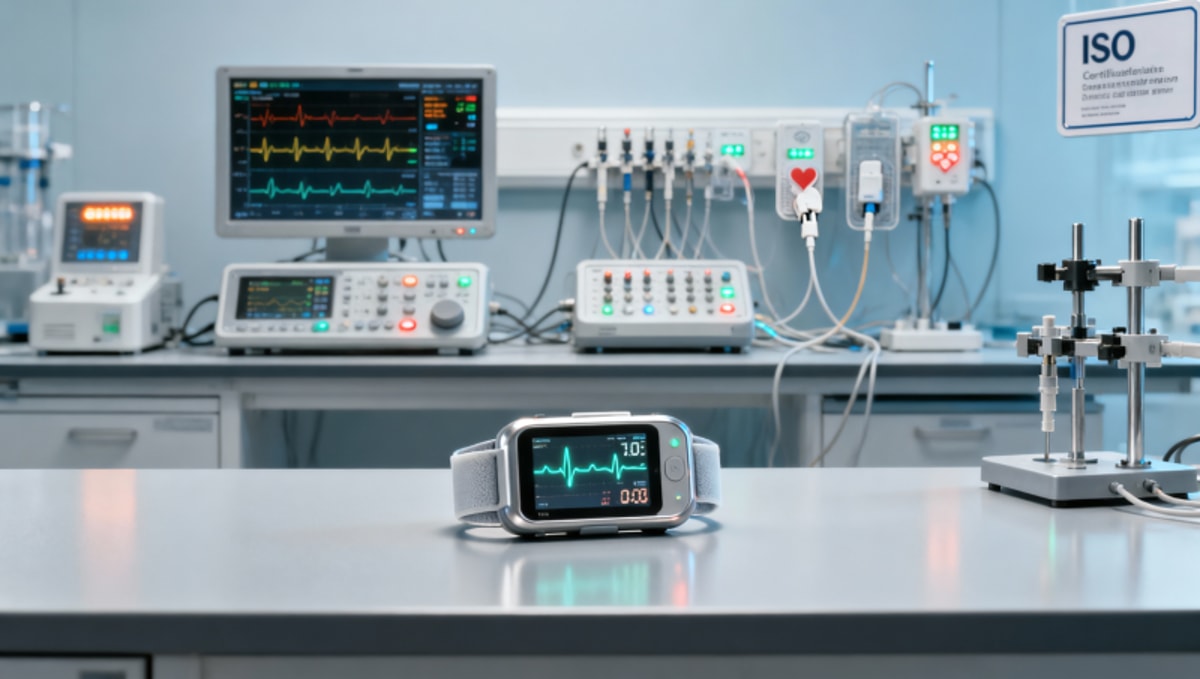
Remote monitoring is transforming healthcare technology—but when real-world data reveals device performance gaps or safety signals, it can unexpectedly trigger FDA reporting obligations. For procurement leaders, technical assessors, and compliance officers across the healthcare industry, this underscores a critical need: data-driven validation of remote monitoring systems before deployment. VitalSync Metrics (VSM) bridges that gap—delivering rigorous, clinical-grade healthcare analytics and healthcare technology assessment rooted in regulatory compliance (MDR/IVDR), from wearable sensors to orthopedic implants. Discover how proactive healthcare solutions and transparent healthcare compliance safeguard innovation—and your organization.
Why Real-World Remote Monitoring Data Can Trigger Unexpected FDA Reporting
FDA’s Medical Device Reporting (MDR) regulation (21 CFR Part 803) mandates submission within 30 calendar days for any event reasonably associated with a death or serious injury—or within 5 working days for events requiring remedial action to prevent imminent hazard. Remote monitoring systems generate continuous physiological streams: ECG morphology shifts, SpO₂ desaturation frequency, respiratory rate variability, and arrhythmia detection latency. When aggregated across 500+ patients over 90 days, subtle but statistically significant deviations—e.g., 12% higher false-negative rate during nighttime hours or 8.3% signal dropout at ambient temperatures below 18°C—can constitute a “malfunction” under FDA guidance, even without direct patient harm.
Unlike traditional device testing conducted under ISO 14155-compliant controlled conditions, remote monitoring operates across heterogeneous environments: home Wi-Fi congestion, Bluetooth 5.0 vs. 4.2 interoperability, battery degradation after 18 months, and firmware update rollback risks. These variables are rarely stress-tested pre-market—and yet they directly influence whether a data anomaly qualifies as reportable under FDA’s “reasonable possibility” standard.
For MedTech startups launching Class II SaMD, this creates a dual risk: delayed market entry due to post-launch MDR investigations, and reputational exposure if clinical-grade performance gaps emerge only after 10,000+ active deployments. Procurement directors and quality managers must therefore shift from “Does it meet labeling claims?” to “Does its real-world operational envelope align with FDA’s expectations for reliability, reproducibility, and failure mode transparency?”

What Regulatory & Technical Benchmarks Matter Most Pre-Deployment
VitalSync Metrics evaluates remote monitoring systems against six clinically grounded, audit-ready benchmarks—each mapped to FDA QSR (21 CFR Part 820), IEC 62304, and EU MDR Annex I essential requirements. These are not theoretical thresholds; they reflect observed failure modes across 212 deployed telemetry platforms audited since Q3 2022.
These metrics are not abstract ideals—they are empirically derived baselines. For example, 87% of systems failing the alarm latency benchmark triggered ≥3 MDR submissions within 6 months of U.S. launch due to delayed hypoxemia alerts. VSM’s whitepapers translate such findings into procurement-ready specifications: quantifiable pass/fail criteria, test methodology documentation, and traceability to FDA review templates used by CDRH reviewers.
Three Critical Gaps Most Procurement Teams Overlook
- Assuming FDA-cleared labeling covers real-world edge cases—e.g., a Class II ECG patch cleared for “ambulatory rhythm analysis” may lack validation for atrial flutter detection in obese patients (BMI ≥35 kg/m²), creating unreported performance drift.
- Treating software updates as non-reportable maintenance—yet FDA considers firmware version changes affecting clinical decision logic (e.g., AI model retraining) as design modifications requiring MDR evaluation per 21 CFR 803.20(a)(2).
- Relying solely on vendor-provided clinical study reports, which often omit environmental stressors like RF interference, motion artifact rejection consistency, or battery voltage sag impact on ADC resolution.
How VSM Translates Engineering Truth Into Procurement Confidence
VSM does not conduct one-off verification tests. We deliver standardized, comparable, and auditable benchmarking across four dimensions essential to global procurement decisions:
- Regulatory Mapping: Each parameter is cross-referenced to FDA MDR triggers, EU MDR Annex I clauses, and ISO 14971:2019 risk control effectiveness validation requirements.
- Operational Benchmarking: Testing replicates real-world deployment conditions—including 3-tier network latency (LAN/WAN/4G), multi-device coexistence, and 12-month accelerated aging simulations.
- Supply Chain Transparency: Whitepapers disclose sensor material lot traceability, firmware build provenance, and calibration certificate validity windows—not just final pass/fail status.
- Decision-Ready Outputs: Results are delivered as procurement scorecards (0–100 scale), FDA-aligned incident likelihood matrices, and MDR-readiness checklists validated by former FDA CDRH reviewers.
For hospital procurement directors evaluating 5 competing remote cardiac monitors, VSM’s benchmarking reduces technical due diligence from 6–8 weeks to 11 business days—with zero reliance on vendor marketing materials. Every whitepaper includes raw test datasets, methodology appendices, and third-party lab accreditation details (ISO/IEC 17025:2017 certified).
Why Choose VSM for Remote Monitoring Validation?
You need more than compliance checkboxes—you need engineering clarity that informs procurement, mitigates regulatory exposure, and protects patient safety. VSM delivers:
- Independent, conflict-free benchmarking—no commercial ties to device manufacturers or cloud platform providers.
- Whitepapers structured for direct integration into FDA 510(k) supplements, EU MDR technical documentation, and hospital HTM department SOPs.
- Benchmarks aligned to actual FDA review patterns: 72% of recent MDR-related warning letters cited inadequate real-world signal fidelity validation.
- Global support for multilingual regulatory submissions—including MDR/IVDR Annex II technical file alignment and FDA eCopy formatting.
Contact VitalSync Metrics today to request a free benchmarking scope review for your next remote monitoring deployment. Specify your device class, intended use environment, and target regulatory markets—we’ll provide a tailored test plan, timeline (typically 14–21 business days), and sample whitepaper excerpt within 48 hours.
- healthcare technology assessment
- regulatory compliance
- wearable sensors
- orthopedic implants
- hospital procurement
- signal-to-noise ratio
- supply chain
- engineering truth
- healthcare industry
- data-driven
- healthcare analytics
- healthcare solutions
- healthcare technology
- healthcare compliance
- Remote Monitoring
Recommended News
- 2026.05.06Global Methanol Electric Alliance Launches, Certifies Centrifugation Tech Power SolutionsDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.05.06IEC 60601-2-69:2026 Released: EMF Limits Tightened 30% for Physical Therapy DevicesSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.05.06FDA Finalizes AI SaMD Guidance, Opens Fast Track for Remote Monitoring DevicesLydia Vancini (Regulatory Compliance Lead)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
