What drives costs in Surgical & Clinical Tech sourcing?
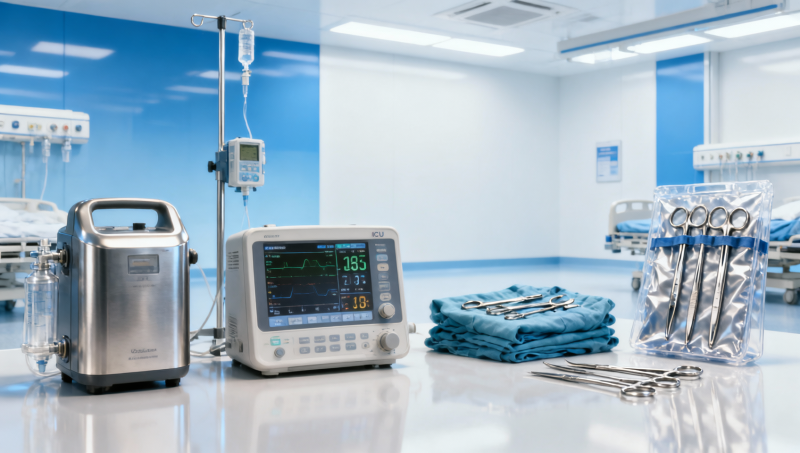
In Surgical & Clinical Tech sourcing, the biggest cost drivers are rarely the quoted unit price alone. For most buyers, the true expense comes from technical verification, regulatory readiness, integration effort, quality consistency, maintenance burden, and the financial impact of downtime or non-compliance. Whether you are evaluating an oxygen concentrator factory, an ICU monitor supplier, or a surgical instrument kits OEM partner, the central question is the same: can this product perform reliably in real clinical settings without creating hidden operational and compliance costs later?
For procurement teams, clinical users, and healthcare decision-makers, this means cost analysis must go beyond price comparison. The most effective sourcing decisions look at total cost of ownership, not just purchase cost. They also test whether a supplier can prove engineering integrity, support digital interoperability, document MDR/IVDR alignment where relevant, and maintain stable performance across production batches.
What is really driving costs in Surgical & Clinical Tech sourcing?
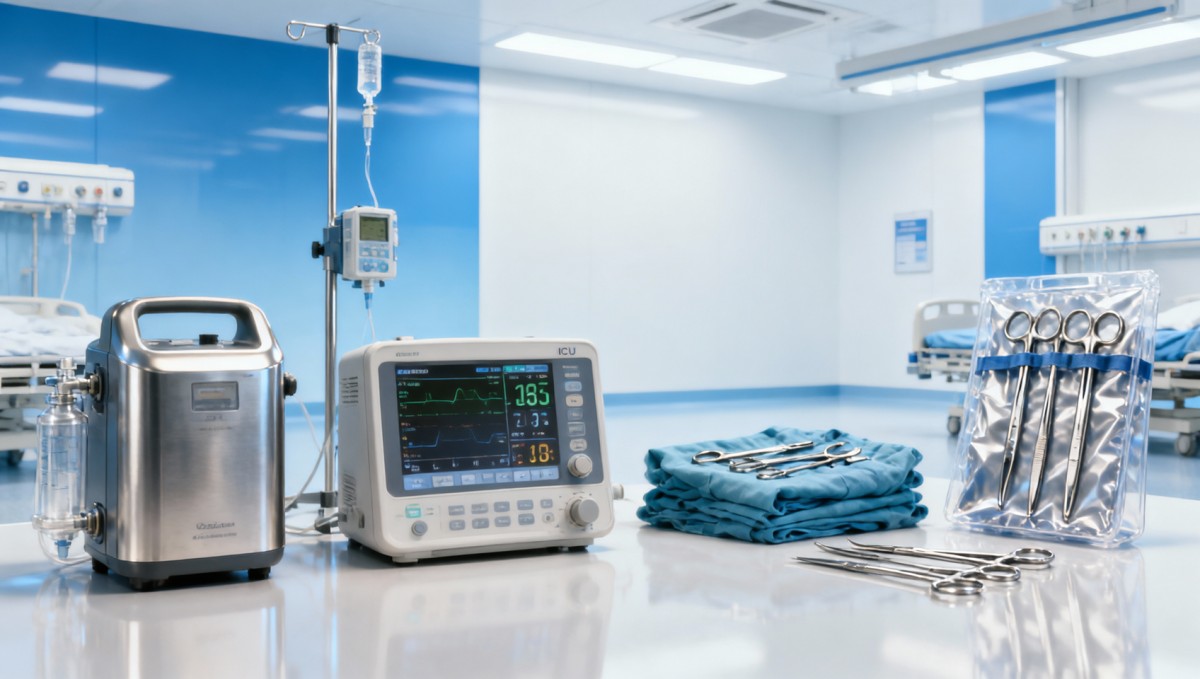
The short answer is this: costs rise when uncertainty rises. In surgical and clinical technology procurement, every unknown has a price. If a supplier cannot clearly demonstrate performance, compliance, traceability, and after-sales capability, the buyer absorbs that risk through added testing, delayed deployment, staff workarounds, or replacement purchasing.
The most common cost drivers include:
- Regulatory compliance requirements such as MDR/IVDR documentation, device classification, labeling, technical files, and audit readiness
- Engineering validation including durability, signal accuracy, calibration stability, material quality, and clinical-grade reliability
- Supplier verification covering factory capability, process consistency, quality systems, and component traceability
- Digital integration complexity with hospital systems, data standards, interoperability expectations, and cybersecurity controls
- Lifecycle service needs such as maintenance, spare parts, training, field support, and software updates
- Failure risk caused by downtime, false readings, sterility issues, rejected batches, or user safety events
- Procurement inefficiency from poor specification alignment, repeated vendor comparisons, and incomplete due diligence
In other words, the farther a product is from verified clinical performance, the more expensive it becomes to source safely.
Why unit price is often the least important number
Many sourcing mistakes begin with a narrow focus on per-unit cost. A lower quote may look attractive during tender evaluation, but clinical technology behaves differently from ordinary industrial goods. If the product requires extra validation, has unstable performance, or generates integration issues, the initial savings disappear quickly.
For example, a low-cost ICU monitor may lead to higher total spend if it causes:
- additional biomedical engineering checks before deployment
- higher alarm inaccuracy or signal noise
- interface problems with central monitoring systems
- staff retraining because workflows are unintuitive
- frequent service interventions or component failure
The same applies to sourcing from an oxygen concentrator factory. The quoted price is only one layer. Buyers also need to understand oxygen purity consistency, compressor durability, maintenance intervals, spare parts access, energy use, and whether the product can sustain expected performance under local environmental conditions.
For surgical instrument kits OEM sourcing, hidden costs often show up in material fatigue, sterilization compatibility, dimensional inconsistency, packaging quality, and the need to replace incomplete or damaged sets. A cheaper kit that fails reprocessing or wears down too quickly is not actually cheaper.
How regulatory and documentation gaps increase sourcing costs
In healthcare, compliance is not a paperwork detail. It is a cost variable. When a supplier lacks complete regulatory documentation or cannot clearly support claims around device classification, intended use, testing evidence, or quality controls, buyers must invest extra time and resources to investigate what should already be proven.
Key cost impacts from weak compliance readiness include:
- Longer qualification cycles because technical and legal teams must request missing documents repeatedly
- Import or market access delays due to incomplete certificates or inconsistent declarations
- Higher audit burden when supplier quality systems are unclear or poorly documented
- Risk of procurement reversal if a selected device later fails review
- Exposure to liability when product claims exceed documented evidence
This is especially relevant in environments shaped by MDR/IVDR expectations, where buyers increasingly need confidence that products are not merely marketable, but technically and clinically defensible. A supplier that can provide structured technical files, validation reports, manufacturing consistency data, and traceability documentation often reduces overall sourcing cost even if the unit price is higher.
Why engineering rigor matters more as medical technology gets more complex
As healthcare equipment becomes smarter, more connected, and more specialized, engineering quality becomes a direct sourcing cost driver. The challenge is no longer simply “does the device work?” but “does it work consistently, under clinical stress, over time, and within a broader healthcare system?”
This is where healthcare engineering rigor changes the economics of procurement. Buyers should assess:
- Performance stability across repeated use and environmental variation
- Signal-to-noise ratio for sensors and monitoring devices
- Material endurance for implants, tools, and reusable instruments
- Calibration drift in diagnostic and measurement systems
- Production repeatability from batch to batch
- Failure mode predictability under real-world usage conditions
If these factors are not verified before purchase, the buyer effectively funds the learning curve after installation. That is one of the most expensive procurement models possible.
Independent benchmarking and technical whitepaper review can be especially useful here because they translate manufacturer claims into measurable decision criteria. For enterprise decision-makers, this reduces uncertainty. For operators and clinical users, it improves trust in what arrives on site.
What hidden supplier-side factors often inflate total cost?
Not all cost drivers are visible in product datasheets. Supplier-side variables often determine whether sourcing remains stable over time or turns into a continuous management problem.
The most important hidden supplier-side factors include:
- Manufacturing process control and the ability to maintain tolerances consistently
- Raw material sourcing quality and documentation depth
- Subcomponent dependency on fragile or geographically concentrated supply chains
- Change control discipline when designs or materials are updated
- Testing methodology transparency and whether acceptance criteria are meaningful
- Scalability if procurement volumes rise after initial approval
- Service response capability in your target market
A supplier may appear cost-competitive at onboarding but become expensive if lead times fluctuate, quality drifts, or support channels are weak. This is why serious surgical and clinical tech sourcing should include supplier capability assessment, not just product comparison.
How digital integration and interoperability affect the cost equation
Clinical technology is increasingly part of a digital ecosystem. Devices that cannot integrate cleanly with electronic medical records, central stations, laboratory systems, or asset management platforms often create hidden implementation costs far beyond hardware pricing.
Common cost drivers tied to digital integration include:
- custom interface development
- middleware requirements
- data mapping and validation work
- cybersecurity hardening
- software version compatibility checks
- user training for hybrid workflows
For example, an ICU monitor supplier may offer attractive hardware pricing, but if the platform does not support the hospital’s interoperability standards or creates alarm management problems, the organization may spend heavily on IT adaptation and workflow correction. In modern procurement, digital compatibility is a cost driver just as real as hardware durability.
What should buyers evaluate before comparing quotes?
For information researchers, procurement teams, operators, and executives, the best way to control costs is to qualify the sourcing decision before negotiating price. A structured pre-quote evaluation helps identify which vendors can truly support long-term value.
Useful evaluation questions include:
- Can the supplier prove clinical-grade performance with test data, not just marketing claims?
- Are MDR/IVDR-related documents, certifications, and technical files complete and current where relevant?
- Is there evidence of stable manufacturing quality and traceability?
- What are the expected maintenance demands and service response times?
- How well will the technology integrate into current workflows and digital systems?
- What failure scenarios are most likely, and what would they cost operationally?
- Can the supplier support scaling, localization, and long-term continuity?
This kind of review turns procurement into risk-managed decision-making instead of reactive price shopping.
How to reduce sourcing costs without sacrificing clinical confidence
The goal is not simply to buy cheaper. It is to reduce avoidable cost while preserving technical and clinical confidence. In practice, that means focusing on verifiable value.
The most effective strategies are:
- Define performance requirements clearly before engaging suppliers
- Use total cost of ownership models instead of unit price alone
- Benchmark technical claims independently whenever possible
- Screen suppliers for process discipline and documentation maturity
- Validate interoperability early rather than after purchase
- Prioritize traceability and change control for critical products
- Include operators and technical users in evaluation to catch workflow and usability risks
This approach is particularly valuable in MedTech and Life Sciences sourcing, where the cost of a wrong decision is amplified by clinical risk, regulatory exposure, and service dependency.
Final takeaway: the biggest cost driver is unverified risk
What drives costs in Surgical & Clinical Tech sourcing? The most accurate answer is unverified risk across compliance, engineering, integration, and supplier reliability. The less evidence a buyer has, the more money the organization will spend compensating for uncertainty later.
For hospitals, laboratories, MedTech startups, and procurement leaders, the smartest sourcing strategy is to look past vendor positioning and focus on measurable proof: technical integrity, regulatory readiness, manufacturing consistency, and lifecycle support. When healthcare equipment is sourced with that level of discipline, procurement becomes more predictable, total cost drops, and long-term clinical performance becomes far easier to trust.
- EMS
- ESS
- PPE
- life sciences
- EdTech
- procurement
- cybersecurity
- AR
- supply chain
- Cement
- material fatigue
- benchmarking
- regulatory compliance
- medical technology
- technical integrity
- material fatigue
- signal-to-noise ratio
- digital integration
- life sciences
- supply chain
- technical verification
- clinical performance
- healthcare engineering
- biomedical engineering
- healthcare equipment
- Packaging
- icu monitor supplier
- surgical instrument kits oem
- oxygen concentrator factory
- life sciences sourcing
Recommended News
- 2026.04.17Hospital equipment standards shaping modern rehab devicesSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.04.17Laboratory equipment validation errors in sample storageDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.04.17Medical equipment certification delays in remote monitoringLydia Vancini (Regulatory Compliance Lead)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
