Why healthcare digital integration breaks at device handoff
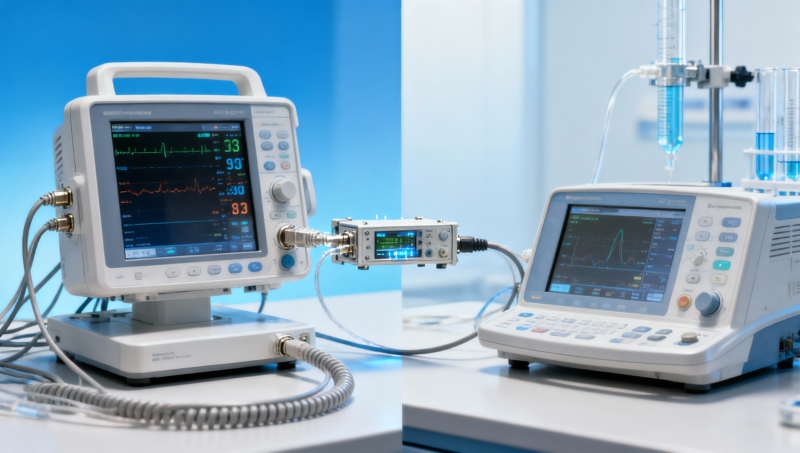
Healthcare digital integration most often breaks at the device handoff because this is where engineering assumptions collide with clinical reality. A device may transmit data, but that does not mean the data is usable, compliant, reliable, or safely embedded into care workflows. For procurement leaders, operators, and healthcare decision-makers, the real issue is not “Can this device connect?” but “Will it perform consistently across systems, users, regulations, and long-term operational demands?” In practice, handoff failures usually stem from weak interoperability design, incomplete medical device evaluation, inconsistent data quality, overlooked workflow friction, and poor MDR/IVDR readiness. Understanding these failure points is essential if hospitals, labs, and MedTech teams want to reduce implementation risk and make sourcing decisions based on measurable technical integrity rather than vendor claims.
Why the device handoff is the most fragile point in healthcare digital integration
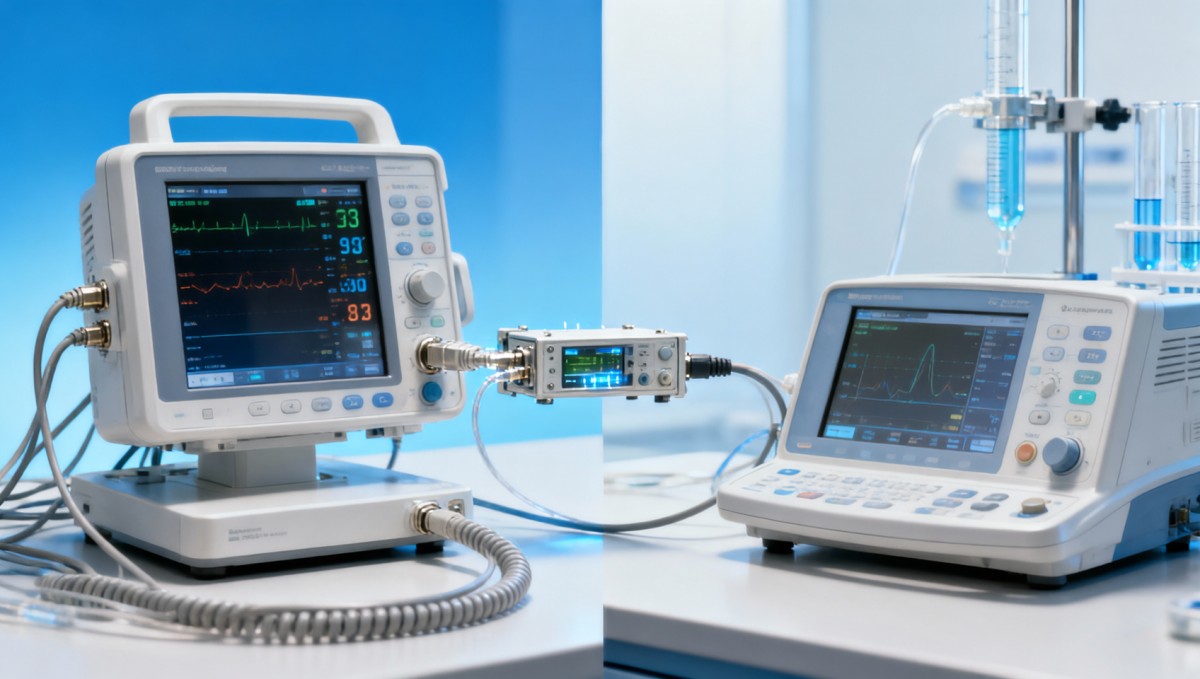
The device handoff is the moment when information leaves a medical device and enters another system, team, or workflow. That transition sounds simple, but it is often where integration breaks down. A wearable sensor, diagnostic instrument, bedside monitor, or connected implant may perform well in a controlled demonstration, yet fail when deployed into a hospital’s real infrastructure.
This happens because healthcare environments are not just technical ecosystems. They are regulated, multi-vendor, workflow-heavy, and highly sensitive to timing, traceability, and patient safety. At handoff, several questions immediately matter:
- Is the output data standardized and interoperable with the receiving system?
- Does the receiving platform interpret values correctly and consistently?
- Can the transfer occur without data loss, duplication, latency, or formatting distortion?
- Is the process compliant with documentation, audit, and regulatory expectations?
- Does the handoff support actual clinician and operator behavior, not just ideal process diagrams?
When the answer to any of these questions is unclear, digital integration becomes fragile. This is why many projects that look successful during procurement or pilot phases later generate operator frustration, missing records, rework, or compliance concerns.
What searchers usually want to know when they ask why integration breaks
Readers searching this topic are rarely looking for a generic definition of interoperability. They usually want a practical explanation of where hidden failure risks sit and how to assess them before those risks become operational or financial problems.
Across information researchers, device users, procurement teams, and executive decision-makers, the most common concerns are:
- Reliability: Will the device-to-system transfer work consistently under real conditions?
- Compliance: Does the product support MDR/IVDR expectations, traceability, validation, and documentation?
- Clinical usability: Will clinicians and operators trust and use the output without creating manual workarounds?
- Procurement risk: Are we buying a device that looks digitally ready but fails after deployment?
- Vendor credibility: Are claims backed by testing, benchmarks, and engineering evidence?
- Total cost: How much hidden integration effort, retraining, troubleshooting, and maintenance will this create?
In other words, the search intent is diagnostic and decision-oriented. People want to understand failure causes so they can evaluate vendors better, protect implementation budgets, and avoid clinical disruption.
The five main reasons healthcare digital integration fails at handoff
1. Data is technically transferred, but not clinically usable. Many systems can send data packets, but the receiving environment may not preserve context, timestamps, units, metadata, alarm meaning, calibration dependencies, or patient linkage. This creates a dangerous illusion of interoperability. Connectivity exists, yet decision-grade information does not.
2. Device performance degrades outside controlled test conditions. Bench performance often differs from real-world performance. Noise, environmental variation, user handling, network instability, battery limitations, middleware behavior, and competing system loads all affect handoff reliability. A device that passes a limited demo may fail under everyday hospital pressure.
3. Workflow design is ignored. Even technically valid integrations fail when they interrupt care delivery. If nurses, lab personnel, or technicians must manually reconcile identifiers, repeat measurements, validate mismatched records, or navigate confusing interfaces, the handoff becomes slow and error-prone. Workflow friction is one of the most common and least acknowledged causes of digital failure.
4. Regulatory readiness is assumed rather than verified. MDR/IVDR readiness is not just a documentation box. It affects risk management, traceability, change control, usability evidence, and lifecycle responsibility. If digital handoff behavior is not properly validated and documented, organizations may inherit compliance exposure long after procurement is complete.
5. Procurement focuses on features instead of engineering evidence. Buyers are often shown dashboards, connectivity claims, and integration promises. What is missing is independent medical device testing, signal quality benchmarking, interface validation, failure-mode analysis, and long-term reliability data. Without these, the handoff risk remains invisible until after installation.
How medical device evaluation exposes hidden integration risk
A strong medical device evaluation process does not stop at headline specifications. It investigates whether the product can maintain performance integrity when data is handed off between systems, departments, and stakeholders.
For healthcare buyers and technical assessors, useful evaluation questions include:
- What interoperability standards are supported, and how completely are they implemented?
- How does the device perform under stress, variable network conditions, or prolonged use?
- What evidence exists for data accuracy after transfer, not just before transfer?
- How are exceptions handled, such as duplicate IDs, missing values, interrupted transmission, or delayed synchronization?
- What validation records support compliance and post-market traceability?
- Has the device been benchmarked independently against comparable systems?
This is where healthcare benchmarking becomes especially valuable. Independent benchmarking can reveal whether a product’s signal fidelity, material durability, latency tolerance, or output consistency holds up beyond vendor-managed conditions. It shifts the conversation from “promised compatibility” to “proven performance.”
For organizations making sourcing decisions across multiple geographies or high-value procurement categories, this engineering-first approach reduces the chance of selecting a device that appears digitally mature but introduces downstream operational risk.
Why operators and clinical teams often see the problem before executives do
Users and operators are usually the first to experience a broken handoff. They are the ones dealing with delayed syncs, repeated entries, missing patient associations, unclear alerts, or inconsistent outputs between device and platform. These issues may seem small individually, but they compound quickly.
From an executive view, a solution may still appear implemented. From the operator view, it is unstable, inefficient, and harder to trust. That gap matters because low-trust systems generate informal workarounds, and workarounds undermine both compliance and data integrity.
Organizations that want better digital integration outcomes should actively collect feedback from the people closest to the handoff point:
- Nurses and bedside operators
- Lab technicians
- Biomedical engineering teams
- IT integration specialists
- Quality and regulatory personnel
If these groups are not involved early in medical device evaluation, procurement decisions may overestimate strategic value and underestimate implementation friction.
What procurement teams should verify before buying connected medical technology
Procurement teams play a critical role in preventing handoff failures. The best sourcing decisions are not driven only by price, brand visibility, or feature lists. They are built on verifiable evidence of technical integrity.
Before selection, procurement leaders should ask for:
- Independent test data on device performance, interoperability behavior, and transfer reliability
- Documented compliance evidence related to MDR/IVDR, validation, risk controls, and lifecycle governance
- Real deployment references in environments similar to their own
- Failure-mode visibility showing what happens when transmission is interrupted or data quality drops
- Maintenance and update transparency including how software changes affect integration stability
- Workflow fit analysis showing the operational impact on users, not just IT architecture
This approach helps decision-makers distinguish between digital marketing maturity and actual healthcare system readiness. In value-based procurement environments, that distinction is financially significant. A lower-cost device with weak handoff reliability may generate higher lifetime costs through downtime, troubleshooting, retraining, compliance exposure, and reduced clinician trust.
How to reduce device handoff failure in practice
Healthcare organizations and MedTech suppliers can reduce integration breakdowns by treating the handoff as a high-risk engineering and workflow event, not a routine technical checkbox.
In practice, that means:
- Test beyond connectivity. Validate data integrity, timing, context preservation, exception handling, and user interpretation.
- Benchmark under realistic conditions. Simulate clinical load, environmental variation, prolonged operation, and multi-system interaction.
- Include operators early. Capture workflow friction before procurement or deployment scales.
- Demand regulatory clarity. Confirm the documentation and validation trail supporting MDR/IVDR and quality management expectations.
- Use independent evidence. Third-party medical device testing and benchmarking provide a more reliable basis for decision-making than self-reported claims.
- Plan for lifecycle performance. Integration success must survive updates, maintenance events, system changes, and long-term use.
For organizations navigating increasingly complex medical technology compliance requirements, this method provides a more resilient path. It supports safer implementation, clearer procurement logic, and stronger long-term return on digital investment.
Conclusion: the real problem is not connection, but trustworthy transfer
Healthcare digital integration breaks at device handoff because that is where technical performance, clinical workflow, compliance obligations, and real-world reliability all converge. The problem is rarely a simple lack of connectivity. More often, it is the failure to verify whether transferred data remains accurate, usable, compliant, and operationally sustainable after it leaves the device.
For information researchers, users, procurement professionals, and enterprise decision-makers, the key takeaway is clear: evaluate the handoff, not just the hardware. The most valuable medical technologies are not the ones that merely claim integration, but the ones that can prove clinical-grade performance through rigorous medical device evaluation, medical device testing, healthcare benchmarking, and documented regulatory readiness. That is how smarter sourcing decisions are made—and how digital healthcare infrastructure becomes safer, more dependable, and genuinely fit for long-term use.
Recommended News
- 2026.06.02Smart Street Lighting Cost-Effective Solutions: Controls, LEDs, and ROILydia Vancini (Regulatory Compliance Lead)
- 2026.06.02Stepper Motors Selection Guide: Torque, Step Angle, Drivers, and Load FitDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.06.02UV Water Sterilizers for Small Facilities: Flow Rate, Dose, and Lamp LifeDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
