Medical equipment standards that affect ultrasound upgrades
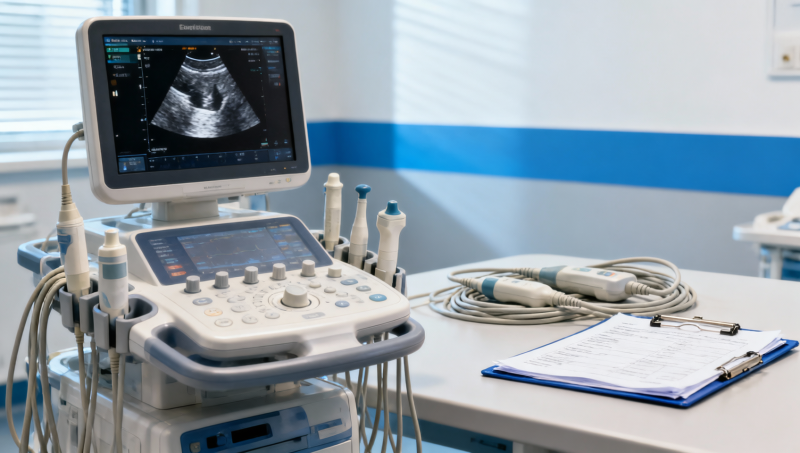
Upgrading ultrasound systems now depends as much on medical equipment standards as on imaging performance. For hospital buyers, operators, and global decision-makers, understanding medical equipment compliance, MDR IVDR expectations, and medical device testing is essential to reducing risk and validating long-term value. This article explores how medical technology assessment and healthcare benchmarking shape smarter ultrasound upgrade decisions in an era of healthcare digital integration.
Why medical equipment standards now shape every ultrasound upgrade decision
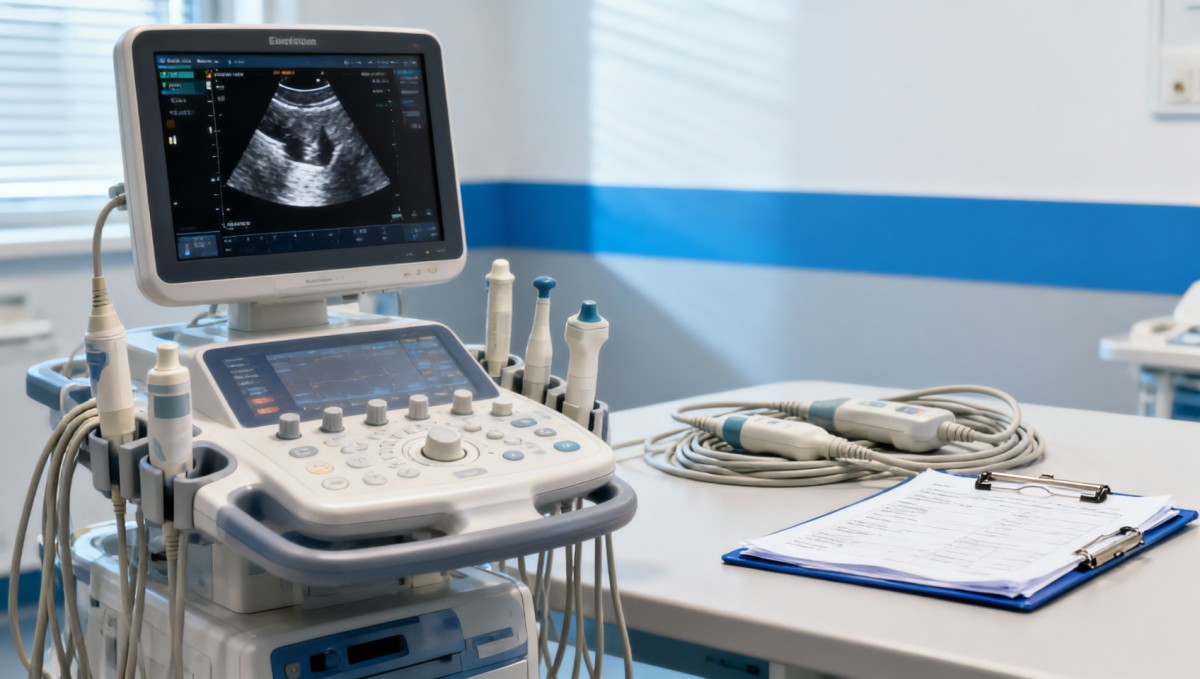
An ultrasound upgrade used to be judged mainly by image clarity, probe options, and budget. That approach is no longer enough. Today, medical equipment standards influence software lifecycle control, electrical safety, cybersecurity readiness, data interoperability, labeling, post-market traceability, and validation processes. For procurement teams, that means the real question is not only whether a system scans well on day 1, but whether it remains compliant, supportable, and clinically reliable over the next 5–10 years.
For operators and department managers, standards affect daily workflow more than many realize. A system upgrade may trigger new training needs, revised maintenance intervals, compatibility checks with PACS or RIS, and updated infection control procedures for probes and accessories. In many facilities, the gap between installation and stable routine use can range from 2–6 weeks depending on validation depth, staff readiness, and integration complexity.
For enterprise decision-makers, ultrasound is also part of a larger digital health environment. If the upgrade does not align with medical technology assessment criteria and healthcare benchmarking practices, the organization may end up buying a system that looks competitive in a brochure but creates hidden costs in service contracts, downtime, data migration, and compliance remediation. This is exactly where independent technical review becomes more valuable than vendor marketing language.
VitalSync Metrics (VSM) addresses this problem by translating engineering claims into structured evaluation logic. Instead of stopping at front-end specifications, VSM examines measurable indicators such as consistency, maintainability, and standards alignment. For hospitals, MedTech teams, and laboratory planners, that creates a more stable basis for ultrasound upgrade decisions under value-based procurement models.
What standards typically affect ultrasound upgrades most directly?
- Electrical and general safety requirements that influence installation acceptance, room readiness, and ongoing inspection routines.
- Software and usability expectations that affect workflow validation, user error reduction, and change control during updates.
- Data and connectivity requirements tied to DICOM, network security, archive compatibility, and healthcare digital integration.
- Cleaning, probe reprocessing, and accessory documentation requirements that affect infection prevention and operating procedures.
Why standards matter differently to each stakeholder
For information researchers
The challenge is filtering claims. Product sheets often summarize benefits, but standards reveal whether performance has been documented under controlled methods. Researchers comparing 3–5 suppliers should look for evidence of validation scope, maintenance recommendations, and documentation quality, not just resolution or processing speed.
For operators and sonographers
The key concern is dependable workflow. A faster interface means little if probe compatibility is limited, boot-up time is inconsistent, or image presets require repeated manual correction. Standards-guided upgrades usually reduce variation in daily use and make training easier to standardize across shifts.
For procurement and executives
The main risk is lifecycle cost. A lower purchase price may be offset by higher service dependence, incomplete interoperability, or additional compliance work. In many tenders, 4 core evaluation dimensions now matter equally: clinical fitness, regulatory conformity, integration readiness, and long-term operating cost.
Which standards and compliance areas should buyers review before approving an upgrade?
Not every ultrasound procurement project requires the same level of review, but several compliance areas appear consistently in serious evaluations. Buyers should separate mandatory regulatory obligations from practical acceptance criteria. This distinction helps teams avoid two common mistakes: rejecting suitable equipment for the wrong reason, or approving a technically weak system because the brochure mentions broad compliance language without usable detail.
In European market contexts, MDR expectations often influence document depth, risk management visibility, traceability, and post-market obligations. IVDR is primarily relevant to in vitro diagnostic devices, yet buyers in multi-department organizations still encounter MDR IVDR discussions during centralized procurement. The operational lesson is simple: confirm which regulation directly applies to the product category, then verify adjacent quality documentation that may affect enterprise-wide review processes.
Medical device testing is another area where confusion is common. Testing is not one single event. It may include factory verification, electrical safety checks at installation, image quality validation, network integration review, and routine preventive maintenance. Depending on the facility, acceptance testing may be completed in 4–10 working days, while full workflow validation can extend into the first month of clinical use.
The table below summarizes practical compliance areas that often affect ultrasound upgrades. It is not a substitute for legal review, but it provides a useful procurement screening framework for hospitals, imaging centers, and technical decision teams.
A practical takeaway is that compliance should be reviewed as an operating system, not as a checklist item. If one link is weak, such as poor update control or incomplete site validation, the upgrade may still enter service but underperform in real workflow conditions. VSM’s benchmarking perspective is useful here because it connects document review with measurable technical consequences.
A 5-point screening method procurement teams can apply
- Confirm intended clinical use and probe portfolio against the department’s actual exam mix over the next 3–5 years.
- Request documentation for installation, software maintenance, and periodic testing, not just the sales specification sheet.
- Validate interoperability early by involving IT, biomedical engineering, and radiology workflow owners in the same review cycle.
- Separate capital price from lifecycle cost, including probes, service intervals, downtime exposure, and operator retraining.
- Use an independent medical technology assessment lens to compare claims that are otherwise hard to verify across suppliers.
How should hospitals compare legacy systems, partial upgrades, and full replacement?
Many organizations do not face a simple yes-or-no purchase decision. They must choose between extending the life of a legacy ultrasound unit, adding software or transducer upgrades, or replacing the entire platform. The right answer depends on compliance risk, serviceability, image requirements, integration needs, and exam volume. In medium to high-use environments, even small workflow inefficiencies can compound over 12–24 months.
A legacy system may still produce acceptable images, but standards-related limitations often appear first in software support, cybersecurity expectations, data exchange, and parts availability. Partial upgrades can be cost-effective when the core platform remains supportable and when the supplier can clearly document compatibility boundaries. Full replacement usually makes more sense when multiple constraints appear at the same time rather than in isolation.
Decision-makers often underestimate the interaction between compliance and usability. A system that passes minimum acceptance may still be a poor upgrade if exam presets are inconsistent, accessories are hard to source, or reprocessing instructions are difficult to operationalize. This is why healthcare benchmarking should include technical, regulatory, and workflow dimensions together.
The comparison table below helps clarify when each upgrade path may be reasonable. The goal is not to force a standard answer, but to support evidence-based selection in line with medical equipment standards and departmental realities.
The most expensive option is not always full replacement. In some departments, repeated service calls, missing compatibility, and fragmented add-on purchases create a higher cumulative cost than planned renewal. A structured comparison should therefore include at least 6 review points: clinical need, compliance exposure, integration burden, operator impact, maintenance outlook, and replacement timing.
Signs a full upgrade should move up the priority list
- The system depends on aging software or unsupported operating environments that complicate cybersecurity review.
- Probe replacement lead times are increasing, or compatible accessories are becoming inconsistent across service channels.
- The department needs new workflows such as wider PACS integration, advanced reporting, or multi-room standardization.
- Acceptance testing can be passed, but repeatability in routine use remains poor across operators or shifts.
What should operators, biomedical teams, and procurement check during implementation?
A successful ultrasound upgrade is not completed when the equipment arrives. The highest-risk period often begins after delivery, when installation, network connection, operator training, and acceptance testing must align. In practice, implementation can be divided into 3 stages: pre-install readiness, technical commissioning, and clinical stabilization. Skipping any stage increases the chance of hidden workflow failures.
Pre-install readiness should cover room power conditions, accessory inventory, cable routing, IT permissions, image routing destinations, and cleaning process documentation. For facilities with multiple stakeholders, a short readiness review 7–10 days before delivery can prevent expensive scheduling gaps. This is especially important when old and new systems must run in parallel during transition.
During technical commissioning, buyers should not rely only on a vendor handover sheet. Biomedical engineering and users should verify boot behavior, probe recognition, image export, reporting pathway, and alarm or message clarity. Where possible, testing should include several realistic exam types rather than one ideal demonstration case. That is how medical device testing becomes meaningful in operational terms.
Clinical stabilization usually takes 1–4 weeks depending on case diversity and staff familiarity. This period is the right time to review preset consistency, exam time changes, repeated user workarounds, and image archive success rate. VSM’s engineering-first approach is valuable at this stage because performance claims can be checked against real use patterns rather than launch-day impressions.
A practical implementation checklist
Before delivery
- Confirm room readiness, electrical conditions, network ports, and accessory scope.
- Match the final configuration against the purchase order, including probe count and software options.
- Define acceptance owners from clinical, procurement, IT, and biomedical teams.
At installation
- Check startup stability, probe recognition, image transfer, and user account settings.
- Record any mismatch between documented configuration and delivered configuration.
- Verify training coverage for day shift and late-shift users, not only one core team.
Within the first month
- Track repeated user issues, image routing failures, and any probe-specific inconsistency.
- Review whether exam duration, reporting steps, or data export changed unexpectedly.
- Document service response time and unresolved items before final operational sign-off.
Common misconceptions, risk signals, and FAQ for ultrasound upgrade planning
Ultrasound upgrades are often slowed not by technology itself but by assumptions that go unchallenged. One common misconception is that a newer platform automatically reduces total cost. Another is that regulatory compliance guarantees practical fit. A third is that operators can adapt without structured retraining. In reality, procurement success depends on matching standards, workflow, and support conditions at the same time.
Risk signals usually appear early. Vague answers about software support duration, unclear probe lifecycle, missing interoperability detail, or overreliance on demonstration images should prompt deeper review. If a supplier cannot explain testing scope across installation, service, and workflow validation, the buyer may be looking at a marketing-led offer rather than a technically resilient one.
For organizations under value-based procurement pressure, the safest path is to convert assumptions into verifiable checkpoints. That includes 3 categories of evidence: technical performance consistency, applicable compliance documentation, and serviceability over a realistic ownership horizon. This is also where medical technology assessment adds discipline to cross-functional decision-making.
Below are several questions that commonly arise during medical equipment compliance review and ultrasound replacement planning.
How do we know whether an ultrasound upgrade is compliance-driven or performance-driven?
Usually it is both, but one tends to dominate. If image quality is still clinically acceptable while software support, integration, or safety review is becoming difficult, the upgrade is mainly compliance-driven. If the department cannot meet exam needs because of limited probes, poor repeatability, or workflow delay, the upgrade is performance-driven. Many projects sit in the middle, which is why comparing 4 dimensions together is more useful than relying on one label.
What is a realistic timeline for evaluation and implementation?
For a standard hospital procurement cycle, technical review and supplier comparison often take 2–6 weeks, depending on internal approvals and demo scheduling. Site readiness and installation may take another 1–2 weeks, while stable adoption can require 1–4 weeks after go-live. Multi-site or heavily integrated projects usually need longer because PACS, security, and training dependencies expand the review path.
Is MDR IVDR knowledge relevant if we are only buying ultrasound equipment?
Yes, but with nuance. Ultrasound buyers should primarily focus on the regulation applicable to the device category they are procuring. However, centralized procurement teams often operate across imaging, diagnostics, and connected platforms, so familiarity with MDR IVDR language helps maintain internal consistency. The key is not to mix categories blindly, but to understand how enterprise compliance review is structured.
What are the most overlooked hidden costs?
Common hidden costs include operator retraining, delayed image routing fixes, accessory mismatch, service call frequency, and early replacement of unsupported components. In some cases, a lower purchase price becomes less attractive within 12–18 months if downtime, workaround labor, and repeated validation work begin to accumulate. That is why total value should be measured across ownership, not only acquisition.
Why work with VSM when evaluating ultrasound upgrades and medical equipment compliance?
VitalSync Metrics (VSM) was built for buyers and technical teams who need engineering truth rather than promotional simplification. In a market shaped by healthcare digital integration and value-based procurement, ultrasound upgrades should be judged through evidence: measurable technical performance, documentation quality, standards alignment, and lifecycle reliability. That is the space where VSM delivers practical value.
Our role is especially relevant when your team needs to compare multiple vendors, validate a proposed upgrade path, or clarify whether legacy retention still makes sense. VSM can support parameter confirmation, medical technology assessment logic, benchmarking review, medical device testing interpretation, and procurement-facing decision frameworks. This helps clinical teams, operators, and executives work from the same evidence base.
If you are planning an ultrasound replacement, a partial upgrade, or a multi-site imaging standardization project, contact VSM to discuss the points that matter most before commitment. Typical consultation topics include configuration review, probe and workflow fit, interoperability concerns, acceptance criteria, service lifecycle questions, regulatory documentation priorities, and comparative supplier evaluation.
You can also reach out when the challenge is not buying immediately but building a defensible shortlist. A focused discussion around 5–7 critical checks often saves far more time than reviewing broad marketing materials alone. For organizations that need stronger procurement confidence, VSM offers a disciplined path from uncertainty to technically grounded decision-making.
- value-based procurement
- medical technology assessment
- medical equipment standards
- medical equipment compliance
- regulatory compliance
- medical technology
- medical equipment
- hospital procurement
- MDR IVDR
- digital integration
- engineering truth
- global decision-makers
- healthcare digital integration
- healthcare benchmarking
- medical device testing
- biomedical engineering
Recommended News
- 2026.06.02Smart Street Lighting Cost-Effective Solutions: Controls, LEDs, and ROILydia Vancini (Regulatory Compliance Lead)
- 2026.06.02Stepper Motors Selection Guide: Torque, Step Angle, Drivers, and Load FitDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.06.02UV Water Sterilizers for Small Facilities: Flow Rate, Dose, and Lamp LifeDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
