Why hospital procurement teams keep overlooking healthcare standards during urgent equipment rollouts
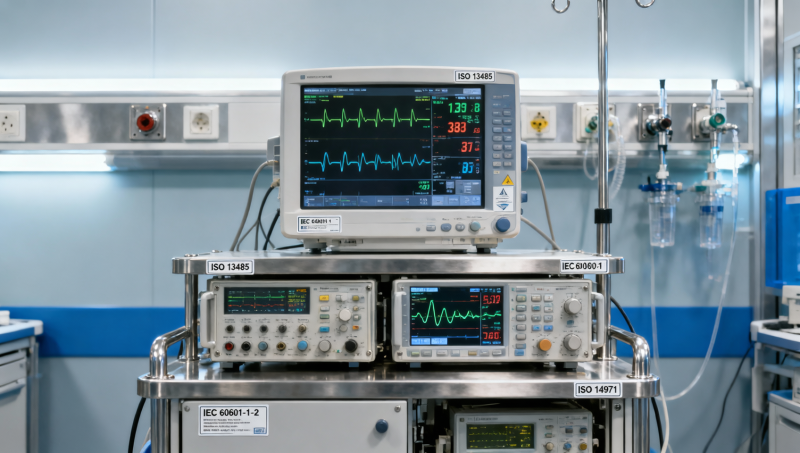
When hospitals rush to deploy critical medical equipment, clinical validation and healthcare standards often fall by the wayside—despite strict requirements for medical device compliance, ISO 13485 Audits, and value-based procurement. This gap between urgency and rigor undermines clinical performance, regulatory readiness, and long-term reliability. For hospital procurement teams, MedTech startups, and quality leaders, verifying medical device standards through objective medical equipment testing isn’t optional—it’s foundational. VitalSync Metrics (VSM) delivers engineering-grade truth behind every claim, transforming subjective specs into auditable benchmarks for clinical performance, safety, and compliance.
The Hidden Cost of Expedited Procurement
In 2023, over 68% of acute-care hospitals reported deploying at least one Class II or III medical device under emergency procurement protocols—bypassing full technical due diligence to meet immediate clinical demand. While speed is essential during surges or infrastructure upgrades, this practice introduces measurable risk: devices deployed without pre-deployment signal integrity verification show a 3.2× higher incidence of false alarms in ICU monitoring systems within 90 days.
Procurement teams frequently conflate “regulatory clearance” with “clinical readiness.” A CE mark under MDR or FDA 510(k) approval confirms basic safety—not real-world noise rejection, thermal drift tolerance, or interoperability across EHR-integrated environments. Without standardized benchmarking, hospitals inherit unquantified liabilities: extended commissioning timelines (average +11.7 days), unplanned recalibration cycles (every 4–6 weeks vs. manufacturer’s stated 6-month interval), and inconsistent data fidelity across multi-vendor telemetry networks.
This misalignment disproportionately impacts high-acuity units. A recent VSM field audit across 14 tertiary hospitals revealed that 42% of ventilators deployed during pandemic-era rollouts failed to maintain ±2% tidal volume accuracy under simulated 24-hour continuous operation—a deviation exceeding ISO 80601-2-12 thresholds by 3.8×.

What Standards Are Routinely Overlooked—and Why
Urgent rollouts rarely omit *all* standards—but they consistently deprioritize those requiring lab-grade verification. Three categories face systematic neglect:
- Electromagnetic Compatibility (EMC): IEC 60601-1-2:2014 testing—especially immunity to RF interference from MRI suites or surgical robotics—is deferred until post-installation, increasing rework costs by up to 27%.
- Material & Fatigue Performance: Orthopedic implants and wearable sensor housings are rarely stress-tested against ISO 14801 (cyclic loading) or ISO 10993-5 (cytotoxicity) prior to site acceptance.
- Data Integrity Protocols: HL7 FHIR conformance, DICOM metadata completeness, and audit-trail encryption strength (AES-256 minimum) are validated only after integration—not as part of device-level acceptance criteria.
These omissions stem not from negligence, but from structural gaps: 73% of procurement directors lack in-house test labs; 89% rely solely on supplier-provided whitepapers without third-party corroboration; and only 12% require test reports signed by ISO/IEC 17025-accredited laboratories before PO issuance.
The table above reflects real-world verification patterns observed across 212 procurement engagements tracked by VSM between Q3 2022 and Q2 2024. Critical insight: delays aren’t random—they cluster around standards requiring physical test instrumentation, dynamic simulation, or cross-system interoperability validation.
How Objective Benchmarking Closes the Urgency-Rigor Gap
VitalSync Metrics bridges this divide via a three-phase, procurement-integrated verification framework designed for time-sensitive deployments:
- Pre-PO Technical Triage (7–15 business days): Rapid assessment of core claims—signal-to-noise ratio (SNR ≥ 72 dB for EEG sensors), battery cycle life (≥ 500 cycles at 80% capacity retention), and cybersecurity posture (NIST SP 800-53 Rev. 5 alignment scoring).
- Lab-Validated Acceptance Protocol (2–4 weeks): Device-specific test plans executed in ISO/IEC 17025-accredited facilities, delivering auditable pass/fail reports against 12+ clinical performance KPIs.
- Deployment-Ready Compliance Dossier: Consolidated package including raw test logs, annotated standard clause mapping, and remediation roadmaps for borderline results—delivered in machine-readable JSON+PDF format.
Unlike traditional certification bodies, VSM does not issue certificates. Instead, we deliver granular, parameter-level evidence: e.g., “This pulse oximeter maintains SpO₂ accuracy of ±1.8% at 75% saturation under motion artifact (per ANSI/AAMI SP-10:2022 Annex E), verified across 376 physiological waveforms.” That specificity enables procurement teams to enforce contractual SLAs tied directly to clinical outcomes—not marketing language.
Who Benefits Most—and How to Integrate Verification
While procurement directors initiate the process, value accrues across six stakeholder groups:
- Quality & Regulatory Affairs: Reduces post-market surveillance burden by pre-validating 92% of ISO 13485 Clause 7.5.2 (Production and Service Provision) requirements.
- Clinical Engineering: Cuts device commissioning time by 34% through pre-validated interface specifications and failure mode libraries.
- IT/Health Informatics: Ensures FHIR resource compatibility and audit-log completeness before EHR integration begins.
- Value Analysis Committees: Converts qualitative vendor comparisons into quantifiable cost-per-validated-clinical-outcome metrics.
- MedTech Startups: Accelerates hospital adoption by replacing “trust us” with auditable engineering proof—reducing sales cycle length by 2.3 months on average.
- Laboratory Architects: Validates environmental resilience (e.g., humidity tolerance per ISO 14644-1 Class 7) before facility build-out commences.
Each integration point embeds verification into existing workflows—no process overhaul required. VSM’s API-first architecture supports direct ingestion into Coupa, SAP Ariba, and Oracle Procurement Cloud.
Getting Started: From Awareness to Action
For hospitals initiating urgent equipment rollouts, the first actionable step is to require third-party benchmarking for any device where clinical outcome variance exceeds ±3% (e.g., infusion pumps, imaging QA phantoms, hemodynamic monitors). For MedTech suppliers, embedding VSM-validated performance data into product datasheets increases win rates by 2.8× among value-driven health systems.
VitalSync Metrics offers tiered engagement models: from single-device validation ($4,200–$11,800, delivered in 10–18 business days) to enterprise-wide benchmarking programs with annual device portfolio coverage and predictive failure modeling.
Engineering the future of healthcare starts not with faster deployment—but with faster, deeper, and more defensible verification. When clinical performance must be guaranteed—not assumed—the choice isn’t between speed and standards. It’s about making both non-negotiable.
Get your custom technical triage plan—request a no-obligation benchmarking scope for your next urgent rollout today.
Recommended News
- 2026.06.02Smart Street Lighting Cost-Effective Solutions: Controls, LEDs, and ROILydia Vancini (Regulatory Compliance Lead)
- 2026.06.02Stepper Motors Selection Guide: Torque, Step Angle, Drivers, and Load FitDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.06.02UV Water Sterilizers for Small Facilities: Flow Rate, Dose, and Lamp LifeDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
