Choosing an ultrasound transducer frequency range for mixed cases
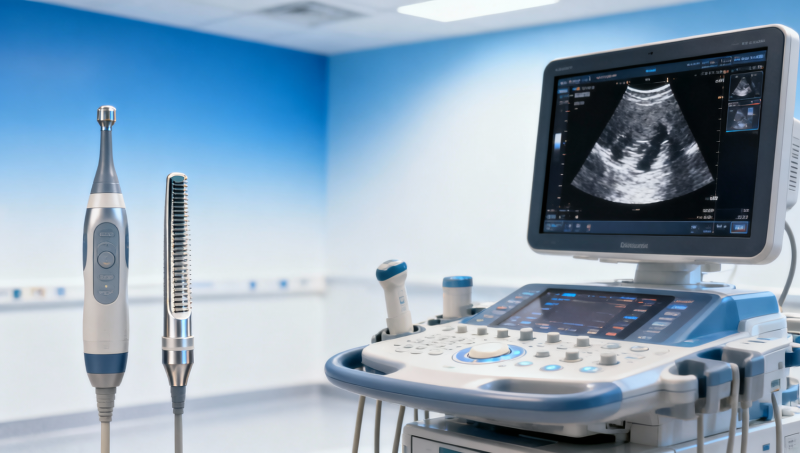
Choosing the right ultrasound transducer frequency range for mixed cases is not just a clinical preference—it is a decision tied to ultrasound metrics, medical device assessment, healthcare compliance, and hospital equipment standards. For operators, buyers, and decision-makers, the short answer is this: there is no single “best” frequency for mixed cases. The right choice depends on your case mix, patient population, image quality thresholds, workflow needs, and how honestly the device performs outside brochure claims. In most mixed-use environments, the practical solution is usually a balanced portfolio approach: a low-to-mid frequency probe for deeper penetration, a higher-frequency probe for superficial detail, and a clear evaluation framework for when one “multi-purpose” transducer is truly enough.
For searchers comparing options, the real question is less about textbook frequency ranges and more about decision quality: How do you choose a probe that works across different exams without sacrificing diagnostic confidence, efficiency, or long-term value? This article focuses on that question from the perspective of users, procurement teams, and healthcare decision-makers who need performance they can verify.
What is the best ultrasound transducer frequency range for mixed cases?
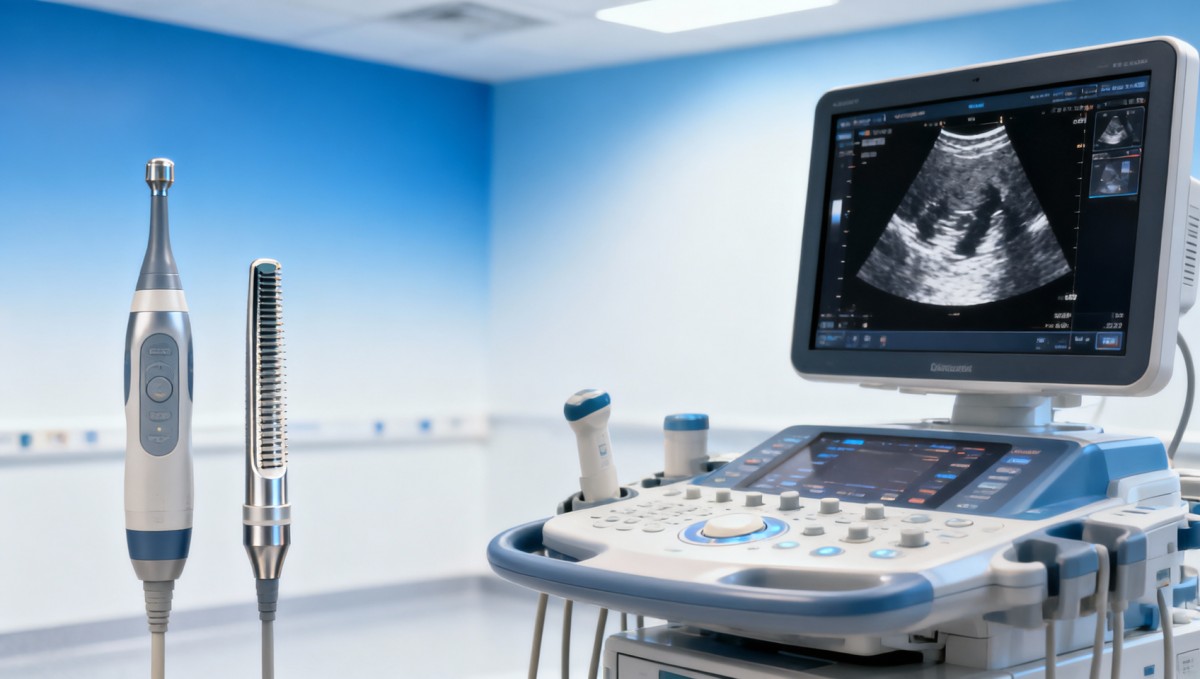
For mixed cases, the most practical frequency strategy is usually to cover both penetration and resolution rather than expect one transducer to do everything equally well.
As a working rule:
- Low frequency (around 2–5 MHz) supports deeper penetration and is commonly preferred for abdominal, obstetric, and deeper pelvic imaging.
- Mid frequency (around 4–9 MHz) often serves as the compromise zone for mixed general imaging, especially where patient body habitus and exam type vary.
- High frequency (around 7–18 MHz or higher) is better for superficial structures such as vascular access, small parts, MSK, breast, thyroid, and soft tissue evaluation where detail matters more than depth.
If your environment truly handles mixed cases—such as a hospital department, outpatient imaging center, or multi-specialty clinic—the best answer is often not a single number but a usable frequency range matched to common indications. In many real-world settings, a convex probe in the low-to-mid range and a linear probe in the mid-to-high range provide the most dependable coverage.
This matters because frequency selection is governed by a simple but decisive trade-off:
- Lower frequency = more penetration, less detail
- Higher frequency = more detail, less penetration
That trade-off becomes critical in mixed cases where operators move between patients with different body types, different anatomical targets, and different diagnostic priorities in the same session.
Why a single “all-purpose” probe often underperforms in real clinical workflow
Many buyers and users search for one transducer that can simplify inventory and reduce cost. That is understandable, but in practice, “all-purpose” claims deserve careful scrutiny.
A broad nominal frequency range printed on a datasheet does not automatically mean the probe delivers consistent image quality across that full range. Some devices market flexible bandwidth, yet their effective performance drops when used at the extremes. In mixed cases, this can create hidden compromises:
- Inadequate penetration in larger or technically difficult patients
- Reduced border definition in superficial anatomy
- Longer scan times due to repeated optimization attempts
- Operator frustration and inconsistency between users
- Increased need for secondary imaging or repeat exams
For operators, this means the probe may technically “work” but not work efficiently or confidently. For procurement teams, this means acquisition cost alone is a poor decision metric. A cheaper transducer that causes workflow delays or inconsistent imaging can become more expensive over time.
The key lesson is that mixed-case suitability should be judged by clinical usability across realistic scenarios, not by marketing language alone.
What operators care about most: penetration, resolution, and speed at the bedside
For sonographers, clinicians, and hands-on users, the frequency decision is usually about whether the probe helps them get a reliable answer quickly.
In daily practice, the most important questions are:
- Can the probe image deep anatomy adequately in larger patients?
- Can it resolve superficial structures clearly enough for confident interpretation?
- How often does the user need to switch probes?
- How much manual optimization is needed to recover acceptable image quality?
- Is performance consistent across routine and difficult cases?
In a mixed-case environment, workflow often matters almost as much as raw image quality. A transducer with theoretically broad frequency coverage may still be a poor choice if it slows the exam, increases adjustment burden, or causes inconsistent results between experienced and less experienced operators.
That is why bedside teams often prefer probe setups that create predictable outcomes:
- A curvilinear probe for abdomen and deeper targets
- A linear probe for superficial, vascular, and procedural use
- In some settings, a phased array probe if cardiac or intercostal access is part of the case mix
From a user perspective, “mixed case readiness” is not just bandwidth—it is the combination of usable depth, acceptable detail, ergonomics, switching logic, and speed.
What procurement and decision-makers should evaluate beyond frequency labels
For buyers, department heads, and enterprise decision-makers, choosing an ultrasound transducer frequency range should be part of a broader medical device assessment process.
The most useful procurement questions are not “What is the widest frequency range?” but:
- What percentage of our actual case mix can this probe cover without compromise?
- What are the failure points in difficult patients or edge cases?
- How does image performance compare under standardized testing?
- Does the probe reduce or increase exam time?
- How durable is the transducer under expected cleaning and usage cycles?
- What service, replacement, and lifecycle costs should be expected?
This is especially relevant in value-based procurement environments. A transducer should be evaluated not only by purchase price, but by its impact on:
- Diagnostic confidence
- Repeat scan rates
- Staff efficiency
- Downtime risk
- Training burden
- Long-term reliability
For organizations seeking defensible purchasing decisions, standardized benchmarking is essential. Independent performance verification can help separate clinically meaningful engineering performance from broad supplier claims.
How to match frequency range to common mixed-case scenarios
A practical selection process starts with the actual exams performed most often. Below is a realistic way to think about common mixed-case patterns.
General imaging department
If the department handles abdomen, pelvic, small parts, vascular, and occasional procedural guidance, a single probe is rarely ideal. A combination of low-to-mid frequency convex imaging plus mid-to-high frequency linear imaging usually offers stronger coverage than one compromise probe.
Emergency and point-of-care settings
In fast-paced settings, versatility is highly valued, but so is immediate usability. A broader-range probe may help reduce switching, yet it must still provide sufficient depth for FAST-style applications and enough detail for vascular access or soft tissue checks. If not, workflow may look simplified on paper but become inefficient in practice.
Outpatient clinics with limited budget
If only one probe can be purchased initially, the best choice depends on the dominant use case. A clinic doing mostly abdominal and OB work should prioritize lower-frequency depth capability. A clinic focused on thyroid, vascular, MSK, or superficial structures should prioritize higher-frequency detail. The right “mixed-case” decision here is really a prioritization decision.
Teaching hospitals and multi-operator environments
Consistency becomes especially important when users have different skill levels. In these environments, a probe that requires extensive manual adjustment may create variability. The better choice is often not the broadest advertised frequency range, but the transducer set that produces repeatable results with less operator dependence.
How to verify whether a transducer really performs across its stated range
Technical claims should be tested against measurable outcomes. Whether you are a hospital buyer, clinical engineer, or department lead, the following checks are more useful than brochure comparison alone:
- Penetration testing: Can the probe maintain usable image quality at clinically relevant depths?
- Resolution assessment: How well does it distinguish small adjacent structures at superficial and moderate depths?
- Uniformity and artifact behavior: Does image quality remain stable across the field?
- Signal-to-noise performance: How much noise appears as depth increases or gain is adjusted?
- Real-case evaluation: How does it perform across different patient sizes and routine indications?
- Ergonomic and handling review: Is the probe practical for prolonged or repetitive use?
- Durability review: How does it tolerate reprocessing, transport, connector stress, and daily wear?
For regulated healthcare environments, this also intersects with compliance and documentation. Procurement teams increasingly need evidence that purchasing decisions align with quality systems, device assessment standards, and risk management expectations. A well-documented evaluation process helps support that requirement.
When should you choose one versatile probe, and when should you buy multiple probes?
A single versatile probe may be reasonable when:
- The case mix is limited rather than truly broad
- Budget constraints are severe
- Workflow strongly favors minimal switching
- The organization accepts moderate performance compromise in non-primary applications
Multiple probes are usually the better choice when:
- The facility manages both deep and superficial imaging routinely
- Diagnostic confidence is a high priority
- Patient body habitus varies widely
- Procedural guidance and specialty imaging are common
- Different departments or users require consistent performance for different tasks
In other words, the decision is not simply clinical—it is operational and financial. A narrow purchase may reduce upfront spend, but if it limits capability, extends exam time, or forces workarounds, the total cost may rise.
A practical decision framework for mixed-case ultrasound transducer selection
If you need a simple way to decide, use this sequence:
- Map your top exam categories by volume and clinical importance.
- Identify required depth and detail thresholds for each category.
- Separate essential performance from nice-to-have flexibility.
- Test probes on representative patient types, not ideal cases only.
- Evaluate operator workflow, including switching frequency and optimization time.
- Review lifecycle factors such as reliability, cleaning, warranty, and replacement cost.
- Document performance evidence for procurement, quality, and compliance purposes.
This approach helps both users and decision-makers avoid an overly simplistic “one range fits all” assumption.
Conclusion: the right frequency range is the one that matches real use, not just specifications
Choosing an ultrasound transducer frequency range for mixed cases is ultimately a matter of matching technical capability to actual clinical demand. The core truth is straightforward: low frequencies help you see deeper, high frequencies help you see finer detail, and mixed cases usually require a deliberate balance rather than a universal setting.
For operators, the best choice is the one that supports fast, reliable imaging across everyday scenarios. For procurement teams and business leaders, the best choice is the one that stands up to standardized assessment, supports workflow, reduces hidden costs, and aligns with quality and compliance expectations.
If you remember one takeaway, let it be this: do not choose based on advertised range alone. Choose based on verified performance, real case mix, and long-term operational value. That is how mixed-case ultrasound selection moves from assumption to informed decision.
Recommended News
- 2026.04.23Low-Altitude Economy Enters Scale-Up Year: eVTOL Infrastructure & Vital Sign SensingLydia Vancini (Regulatory Compliance Lead)
- 2026.04.23Lianyirong, ABC Shanghai Dongfang Hub Branch Close Two e-NI TransactionsDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.04.23China’s April 2026 LPR Set at 3.0% (1Y) and 3.5% (5Y+): Implications for Medical Device Export Financing
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
