Why Ultrasound Metrics vary across the same imaging exam
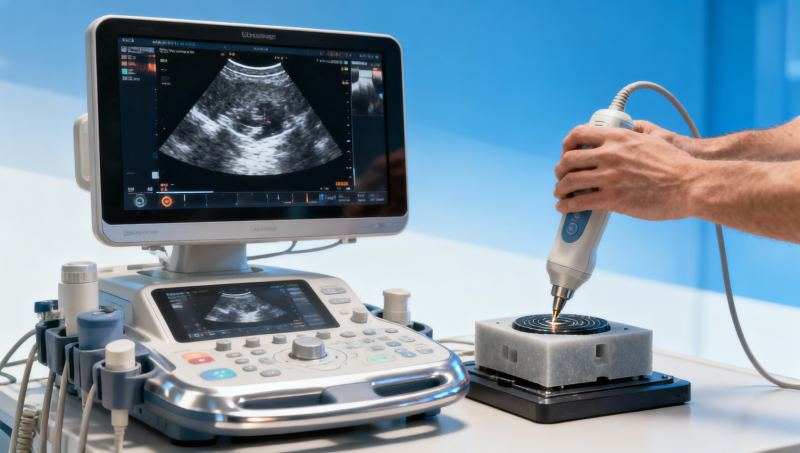
Why do Ultrasound Metrics shift within the same imaging exam? For procurement teams, operators, and decision-makers, these variations affect medical device assessment, healthcare compliance, and trust in clinical performance. This introduction explores how ultrasound transducer frequency range, calibration drift, operator technique, and medical equipment standards influence repeatability—helping buyers and users evaluate data with greater confidence.
In practical healthcare settings, a single ultrasound session can produce measurable differences in signal intensity, depth penetration, edge definition, and derived quantitative values. These changes may happen within 5 to 20 minutes, even when the same patient, probe, and machine are involved. For hospitals and MedTech buyers, the issue is not only clinical interpretation. It also affects acceptance testing, vendor comparison, service planning, and long-term performance verification.
For organizations working under value-based procurement and regulatory oversight, the key question is not whether variation exists, but whether the variation remains within a controlled and explainable range. This is where engineering-based benchmarking becomes essential. Instead of relying on brochure claims, decision-makers need traceable performance data, repeatability checks, and a clear understanding of what causes instability during the same imaging exam.
Why metric variation happens even during one ultrasound exam
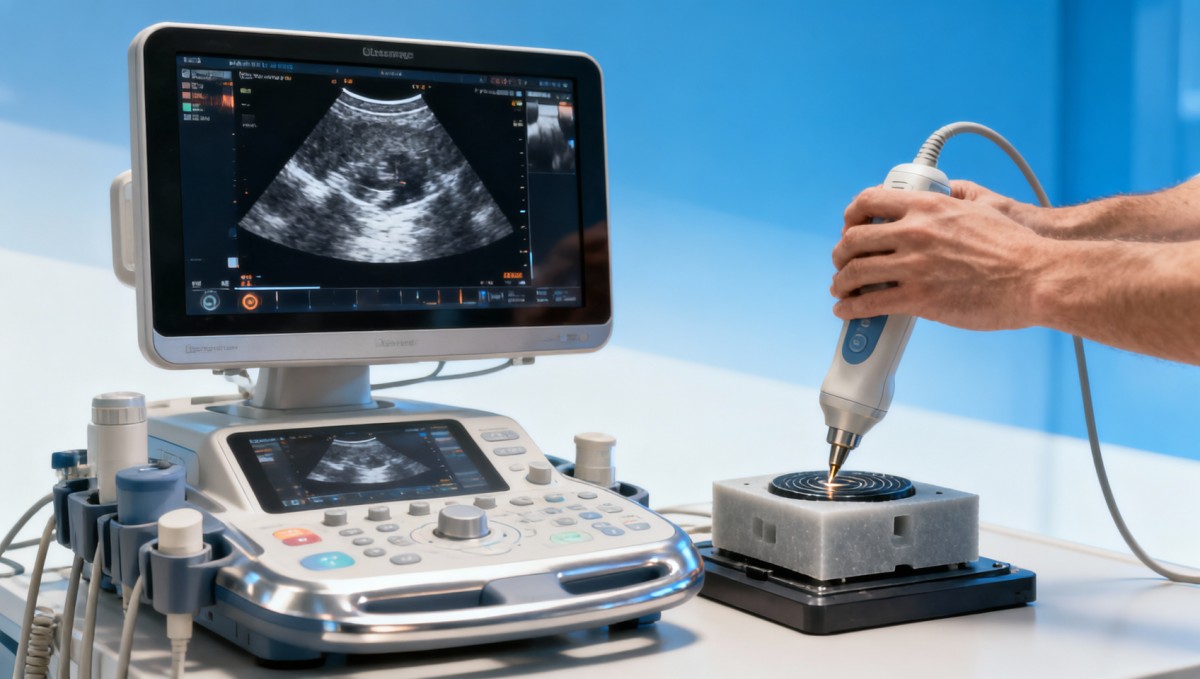
Ultrasound systems do not generate fixed outputs in the way a static ruler measures length. They create images and metrics through an interaction of acoustic energy, tissue properties, electronics, software processing, and operator input. A 3 MHz to 12 MHz transducer, for example, behaves differently at shallow and deep targets, and small adjustments in gain, dynamic range, focal zones, or probe pressure can shift measurable results within seconds.
Probe frequency is one of the first variables to consider. Lower-frequency scanning, such as 2 to 5 MHz, usually improves penetration but reduces fine detail. Higher-frequency scanning, such as 7 to 15 MHz, improves superficial resolution but becomes more sensitive to attenuation. If the exam involves switching presets or adaptive imaging algorithms, the reported ultrasound metrics may vary even without obvious image degradation to the human eye.
Another common source is thermal and electronic drift. After startup, some systems need 10 to 30 minutes to reach stable operating conditions. During this period, transmit power, receiver sensitivity, and internal reference behavior may settle. In high-throughput departments, machines can run continuously for 6 to 10 hours, and heat buildup may alter consistency if preventive maintenance and cooling pathways are not managed properly.
Patient-side factors also matter. Breathing motion, tissue compression, body habitus, bowel gas, and hydration state can alter the acoustic path. In repeat sweeps over the same anatomy, even a 2 to 3 mm change in transducer angle may affect Doppler angle correction, lesion border recognition, or elastography output. From a procurement perspective, this means system stability must be assessed together with workflow realism, not under idealized lab-only conditions.
Core mechanisms behind short-interval variability
Within the same exam, variability often emerges from four combined mechanisms rather than one isolated defect. Hospitals that understand these mechanisms are better equipped to distinguish normal operating ranges from unacceptable performance drift.
- Acoustic factors: attenuation, reflection, refraction, and focal mismatch change returned signal strength.
- System factors: calibration drift, firmware processing, beamforming logic, and temperature-related electronic changes influence repeatability.
- Human factors: probe pressure, insonation angle, ROI placement, and preset selection alter measurements.
- Workflow factors: patient repositioning, exam duration, accessory use, and room conditions such as 18°C to 24°C temperature range affect consistency.
The table below summarizes the most common causes of variation and how they typically appear during technical review or clinical operation.
The key takeaway is that ultrasound metrics vary for understandable engineering and procedural reasons. A stable system does not eliminate all fluctuation; it limits unexplained fluctuation to a manageable range and provides enough transparency for technical validation.
How operators and users influence repeatability in daily workflow
Operator technique remains one of the strongest influences on ultrasound repeatability. Even on premium equipment, image-derived values can drift when exam steps are not standardized. In many departments, 3 to 5 sonographers may use the same platform across different shifts. Without protocol alignment, one user may increase gain to visualize weak echoes while another adjusts depth or focus, producing metrics that are technically valid but not directly comparable.
Probe handling is especially important. Excessive pressure can compress superficial tissue and alter apparent lesion dimensions, vascular signals, or elastography stiffness values. Too little pressure can reduce contact quality and increase artifacts. For small-part, vascular, and musculoskeletal applications, a subtle difference in hand position maintained over 20 to 40 seconds can change the outcome more than many users expect.
Another issue is ROI placement. Quantitative measurements such as spectral Doppler velocity, intima-media thickness, strain ratios, or grayscale histogram analysis depend on consistent sampling zones. A 1 to 2 mm shift in sample volume or boundary selection may be acceptable in routine care, yet problematic in benchmarking, device comparison, or follow-up protocols where tighter repeatability is required.
Workflow controls that reduce user-driven variability
User variability can be reduced through procedural controls rather than relying only on individual experience. This matters for both clinical operators and procurement teams validating multi-site performance before a system-wide rollout.
- Define one approved preset per target application, with locked or documented changes for gain, depth, focus, and dynamic range.
- Use a standard warm-up window, often 15 to 20 minutes, before acceptance testing or quantitative studies.
- Train users on probe pressure, insonation angle, and ROI placement with competency checks every 6 to 12 months.
- Repeat critical measurements at least 3 times and document the average plus range instead of relying on a single capture.
- Audit inter-operator variability by comparing the same phantom or protocol across at least 2 operators.
When “same exam” does not mean “same conditions”
It is common to assume that one imaging session represents a fixed environment. In reality, micro-variations accumulate quickly. The patient may inhale more deeply, the operator may re-angle the probe, automatic optimization may update the image chain, or the sonographer may freeze and remeasure using a different frame. Each step can alter the recorded metric without indicating device failure.
For users, the practical goal is not perfect identity between every frame. The goal is controlled reproducibility within clinically and technically acceptable limits. For procurement and quality teams, this means training plans should be reviewed alongside hardware specifications and service agreements.
What procurement teams should verify before trusting ultrasound performance claims
Procurement teams often receive performance statements framed around image clarity, advanced software, or broad application coverage. These points are useful, but they do not answer the deeper question: how stable are ultrasound metrics over repeated use, across operators, and through the system lifecycle? A sound purchasing decision should examine evidence generated under realistic operating conditions, not only showroom demonstrations.
In regulated healthcare environments, procurement should connect technical performance with compliance and serviceability. For systems entering EU-aligned pathways, teams may review documentation relevant to MDR or IVDR-linked workflows where measurement integrity, traceability, and post-market monitoring matter. Even where ultrasound itself is not judged under one single metric, the consistency of outputs still affects clinical confidence, audit readiness, and downstream integration into digital records or analytical platforms.
A robust tender or evaluation process should include phantom-based repeatability, operator comparison, service response criteria, and calibration history expectations. If a vendor cannot explain drift thresholds, test conditions, or maintenance intervals, the organization may inherit hidden lifecycle costs 12 to 36 months after deployment.
A practical evaluation framework for buyers
The following table provides a procurement-oriented framework that links technical questions to business risk and implementation value.
This approach shifts procurement from feature buying to evidence-based sourcing. It also aligns with the mission of technical benchmarking organizations such as VitalSync Metrics, where the objective is to translate engineering reality into decision-ready data.
Key red flags during vendor evaluation
- No clear test protocol for repeated measurements within the same exam window.
- Performance claims based only on ideal lab snapshots rather than routine-use conditions.
- Undefined service intervals or no explanation of how probe degradation is monitored.
- Limited documentation on software version control, update effects, or exported measurement consistency.
When these red flags appear, buyers should request independent benchmarking or third-party technical review before committing to a fleet purchase, especially for multi-site deployments or specialized imaging programs.
Standards, benchmarking, and engineering controls that improve confidence
Confidence in ultrasound metrics is built through measurement discipline. This includes acceptance testing, scheduled quality assurance, controlled phantoms, software traceability, and documented environmental conditions. In practice, many organizations perform routine QA monthly or quarterly, while full technical review may occur annually or after a major repair, probe replacement, or software upgrade.
Benchmarking should focus on repeatability, not just peak image quality. A system that performs impressively in one demonstration but produces wider variance over 10 repeated scans may be less suitable for longitudinal follow-up, quantitative workflows, or procurement frameworks that prioritize lifecycle reliability. Engineering controls should therefore include pre-defined acceptance bands, consistent test objects, and version-controlled protocols.
Environmental stability is often underestimated. Room temperature shifts of 3°C to 5°C, poor cable handling, probe face wear, and inconsistent power quality can all influence signal behavior over time. While these factors may not immediately produce a visible failure, they can widen variability enough to complicate technical validation and user trust.
Recommended control points for technical teams
The table below outlines practical control points that healthcare engineering teams, laboratory architects, and procurement stakeholders can use during benchmarking and post-installation verification.
These control points are especially valuable when organizations need to compare systems from different vendors, support digital integration projects, or publish internal whitepapers that convert technical findings into procurement-ready conclusions.
Why independent benchmarking matters
An independent benchmarking model helps separate engineering truth from commercial positioning. For decision-makers, that means clearer visibility into what is normal variance, what is operator-related, and what may indicate design or maintenance weakness. For MedTech startups and supply chain partners, it creates a more credible path to technical validation when approaching hospitals, laboratories, or global distribution channels.
Practical selection, implementation, and FAQ for decision-makers
Selecting an ultrasound platform should combine clinical fit, technical repeatability, service structure, and documentation quality. A strong implementation plan usually spans 4 stages: pre-purchase evaluation, acceptance testing, user training, and ongoing quality review. This structure is more reliable than purchasing on image appearance alone, especially when systems will be used across radiology, point-of-care, vascular, or specialty departments.
For healthcare organizations under budget pressure, the right question is not simply whether one unit costs less at purchase. A lower upfront price can become more expensive if drift checks are unclear, probes fail early, or repeated measurements require more rescans and operator time. Over a 3- to 5-year period, repeatability and service responsiveness often matter as much as acquisition price.
Implementation checklist
- Define 4 to 6 acceptance criteria before delivery, including image uniformity, repeatability, probe integrity, export performance, and service documentation.
- Run baseline testing with one phantom and at least 2 trained users within the first installation week.
- Document software version, preset library, and calibration records on day 1 to support later comparisons.
- Schedule refresher training every 6 to 12 months for high-turnover departments.
- Plan a post-update verification workflow whenever firmware or probes are changed.
FAQ
How much variation is acceptable within the same imaging exam?
There is no universal single threshold because acceptable variation depends on the metric, anatomy, workflow, and clinical purpose. In procurement and QA practice, the more useful approach is to define an internal repeatability band for each application, based on repeated scans under controlled conditions, rather than assume one fixed number fits every department.
Does a changing metric always mean the ultrasound system is faulty?
No. Variation may result from operator technique, patient motion, preset changes, or thermal stabilization. A fault becomes more likely when drift is persistent, unexplained, increasing over time, or linked to probe damage, failed calibration, or inconsistent outputs under repeated phantom testing.
What should procurement teams ask vendors before purchase?
Ask for repeated-measurement evidence, warm-up requirements, service intervals, software version control process, probe durability guidance, and post-repair verification methods. Also request a realistic service response commitment, such as 24 to 72 hours for critical support, and evidence of how user training is handled after installation.
How often should repeatability be reviewed after installation?
A common approach is monthly or quarterly routine checks, with additional verification after software updates, major repairs, probe exchange, or sudden shifts in user feedback. High-volume departments may require more frequent review than low-utilization sites.
Understanding why ultrasound metrics vary across the same imaging exam is essential for clinicians, operators, procurement teams, and executive decision-makers. The issue sits at the intersection of engineering behavior, user technique, maintenance discipline, and compliance readiness. Organizations that evaluate repeatability in a structured way are better positioned to reduce risk, compare vendors fairly, and protect trust in clinical performance.
VitalSync Metrics supports this need by turning technical complexity into clear benchmarking logic for the MedTech and Life Sciences supply chain. If you need a more rigorous framework for ultrasound performance evaluation, supplier comparison, or technical whitepaper development, contact us to discuss your use case, request a customized assessment approach, or explore broader healthcare benchmarking solutions.
- EMS
- ESS
- PPE
- life sciences
- EdTech
- procurement
- AR
- supply chain
- Cement
- benchmarking
- value-based procurement
- medical device assessment
- medical equipment standards
- medical equipment
- technical benchmarking
- digital integration
- life sciences
- supply chain
- engineering truth
- clinical performance
- healthcare engineering
- healthcare benchmarking
- healthcare compliance
- Ultrasound Metrics
- ultrasound transducer frequency range
Recommended News
- 2026.04.21Medical equipment standards keep shifting across export marketsDr. Julian Rossi (RehabTech Specialist)
- 2026.04.21Surgical robot latency test results can mislead without contextDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.04.21How much surgical robot latency test time is too much?Dr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
