Hospital equipment standards that affect maintenance planning

Hospital equipment standards have a direct impact on how hospitals plan maintenance, allocate budgets, qualify suppliers, and manage clinical risk. In practice, standards do far more than define product safety at the point of purchase: they influence preventive maintenance intervals, calibration needs, documentation requirements, spare-parts strategy, software update controls, and decisions about repair versus replacement. For procurement teams, equipment users, and healthcare leaders, the key question is not simply whether a device is compliant, but how standards such as MDR-related requirements, electrical safety rules, quality system expectations, and medical device assessment criteria affect long-term serviceability and operational uptime.
For organizations managing Surgical & Clinical Tech, Laboratory & Life Sciences systems, or Rehabilitation & Bionics equipment, the smartest maintenance planning starts with a standards-based view of the asset lifecycle. That means understanding which standards apply, what evidence suppliers can provide, how those requirements translate into maintenance tasks, and where noncompliance can create hidden cost, downtime, or patient safety exposure.
Why hospital equipment standards matter so much in maintenance planning
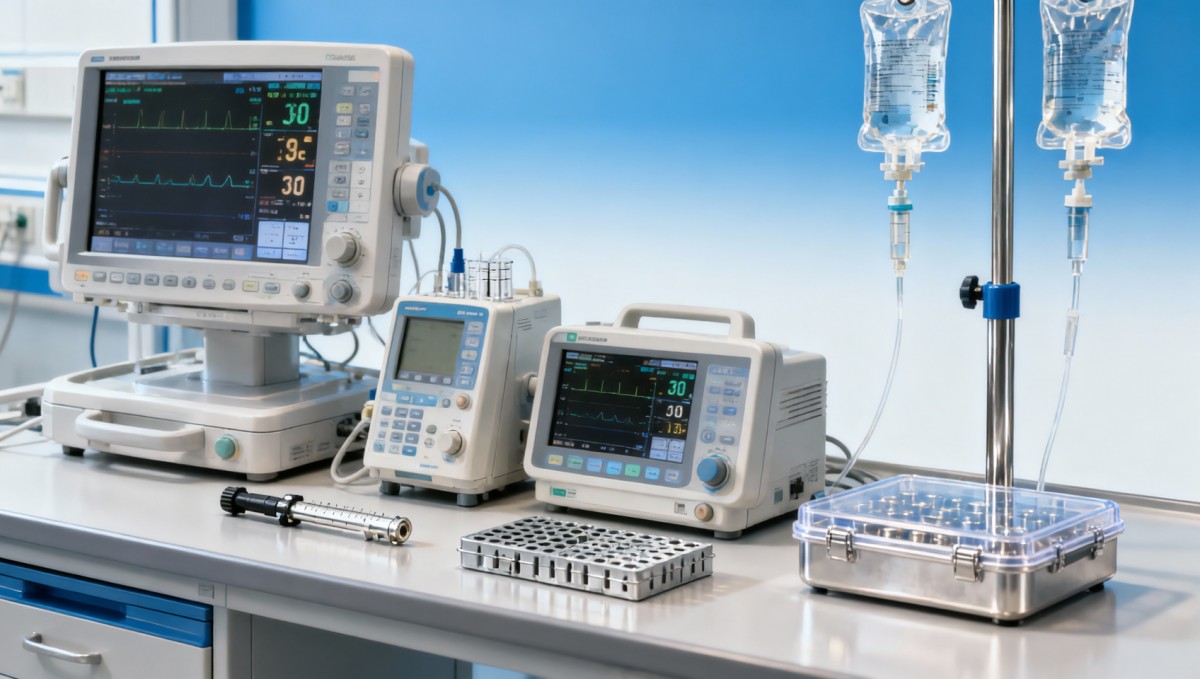
The core search intent behind this topic is practical: readers want to know which hospital equipment standards actually affect maintenance planning and how those standards change day-to-day decisions. They are usually not looking for a purely academic list of regulations. Instead, they want to understand what to check before procurement, what maintenance teams must document, and how standards affect cost, uptime, and risk.
In healthcare environments, maintenance planning is shaped by several overlapping obligations:
- Patient and operator safety — equipment must perform within defined safety and functional limits.
- Regulatory compliance — maintenance activities must not compromise certified performance or intended use.
- Clinical continuity — hospitals need reliable uptime for critical systems.
- Audit readiness — service records, calibration logs, and change controls must stand up to internal and external review.
- Lifecycle cost control — maintenance plans must reduce avoidable failure without overservicing assets.
This is why hospital equipment standards are not just an engineering issue. They influence procurement criteria, technician training, spare-part approval, software servicing, cybersecurity review, and capital replacement planning.
Which standards most often affect hospital maintenance plans
Different device categories are governed by different frameworks, but several standards and compliance domains repeatedly affect maintenance planning across healthcare facilities.
1. Medical device regulatory frameworks such as MDR
For organizations operating in or sourcing into regulated markets, MDR certification and related medical device assessment processes are highly relevant. These frameworks affect maintenance because any servicing activity must preserve the device’s validated safety and performance profile. If repairs, part substitutions, firmware changes, or third-party interventions alter intended performance, the hospital may inherit compliance risk.
Maintenance implications include:
- Using approved service procedures and qualified parts
- Controlling post-service functional verification
- Tracking device modifications and software updates
- Ensuring documentation supports auditability
2. Electrical safety and electromagnetic compatibility standards
For many classes of hospital equipment, standards related to electrical safety and EMC directly determine inspection frequency, test methods, and service acceptance criteria. Devices such as patient monitors, infusion systems, imaging accessories, analyzers, and rehabilitation electronics may require periodic safety verification after installation, repair, or relocation.
These standards often drive:
- Leakage current and grounding tests
- Power quality and insulation checks
- Verification after component replacement
- Environmental suitability reviews in clinical areas
3. Calibration and metrology requirements
Laboratory equipment, diagnostic systems, sensors, and measurement-based devices are heavily influenced by calibration standards. Maintenance planning for these assets must include accuracy verification, traceability, calibration intervals, and out-of-tolerance response procedures. Without this, clinical or laboratory results may become unreliable even if the device appears operational.
4. Quality management and service documentation requirements
While hospitals are not manufacturers, supplier quality systems and service documentation discipline strongly affect maintenance outcomes. A device supported by robust service manuals, spare-parts traceability, revision-controlled documentation, and formal complaint handling is easier to maintain safely over time. Weak documentation often increases downtime and makes maintenance planning reactive rather than controlled.
5. Cybersecurity and software lifecycle controls
Modern connected medical systems increasingly require maintenance plans that include software patch review, access control, update validation, and network-related risk management. For digital and connected devices, maintenance is no longer only mechanical or electrical. Standards and guidance around secure servicing now affect service scheduling and approval workflows.
What procurement teams should evaluate before purchase if maintenance is a priority
Many maintenance problems begin during procurement. A compliant device can still be expensive or difficult to maintain if serviceability was never properly assessed. Procurement teams should therefore expand evaluation beyond product specifications and price.
Questions that matter include:
- What standards does the device claim conformity to? Request clear evidence, not only marketing statements.
- What does the medical device assessment documentation show? Look for validated performance boundaries, service conditions, and post-market obligations.
- Are maintenance intervals fixed, usage-based, or condition-based? This affects staffing and total cost.
- Can the hospital perform first-line maintenance internally? Or is OEM-only servicing required?
- Are spare parts, consumables, and calibrated tools readily available?
- How are software updates controlled? Unclear update policies create compliance and uptime risk.
- What post-repair testing is mandatory? This can significantly affect turnaround time.
- Is there a documented end-of-support timeline? This is critical for replacement planning.
For enterprise decision-makers, these questions help separate low-price acquisitions from low-risk, maintainable assets. In value-based procurement, the most economical device is often the one with the clearest compliance evidence, strongest engineering documentation, and most predictable service model.
How standards change maintenance planning in real operational terms
Standards become meaningful when they change actual maintenance planning decisions. In hospital operations, this usually affects five core areas.
Maintenance frequency
Standards and manufacturer instructions help define whether equipment needs scheduled preventive maintenance, periodic inspection, calibration, functional verification, or event-based testing after repairs or relocation. Critical care and diagnostic devices often require more formal service controls than lower-risk support equipment.
Maintenance scope
Not all maintenance is equal. Some standards-driven tasks are limited to cleaning, lubrication, and visual inspection. Others require electrical safety testing, sensor recalibration, alarm verification, software integrity checks, or validation against defined tolerances. Planning must reflect this difference.
Competency requirements
Standards may indirectly determine who is allowed to perform maintenance. Some actions can be handled by in-house biomedical teams, while others require OEM-trained personnel or certified specialists. This affects labor planning, service contracts, and response time.
Documentation and traceability
In a regulated healthcare environment, undocumented maintenance is often treated as maintenance that did not happen. Standards-linked documentation usually includes service dates, parts replaced, test results, calibration records, deviations, approvals, and release-to-use confirmation.
Replacement timing
Standards do not just affect maintenance; they also shape retirement decisions. If equipment can no longer be maintained to certified performance, if supported parts are unavailable, or if software and cybersecurity requirements can no longer be met, replacement becomes a compliance and operational necessity rather than a discretionary budget item.
Common risks when hospitals ignore standards in maintenance planning
Organizations that treat maintenance as a generic technical function often overlook standards until a failure, audit issue, or procurement dispute exposes the gap. The most common risks include:
- Unexpected downtime due to missing preventive tasks or unavailable approved parts
- Failed audits because service documentation does not support compliance claims
- Clinical performance drift in devices that require calibration or verification
- Increased service costs from reactive repairs and emergency vendor dependence
- Patient safety exposure where post-maintenance testing is incomplete or inconsistent
- Procurement regret when equipment is technically compliant but operationally difficult to support
These risks are especially relevant in complex environments where hospitals manage mixed fleets across different manufacturers, aging platforms, and digitally connected systems.
A practical framework for standards-based maintenance planning
For readers looking for a usable approach, a standards-based maintenance plan can be built around a few practical steps.
- Classify assets by clinical criticality and risk. High-impact assets need stricter maintenance controls and faster service response.
- Map applicable standards and regulatory obligations. Include safety, calibration, software, and device-specific requirements.
- Collect supplier evidence. Verify conformity declarations, service manuals, maintenance schedules, test procedures, and MDR-related documentation where relevant.
- Define maintenance tasks by asset type. Separate routine inspection, preventive maintenance, calibration, and post-repair validation.
- Assign responsibility. Clarify what users, in-house technicians, third-party providers, and OEMs are each allowed to do.
- Set documentation rules. Ensure every intervention is traceable and reviewable.
- Link maintenance data to procurement and replacement decisions. Repeated failures, support limitations, and standards-related issues should inform future sourcing.
This framework helps both technical teams and managers move from checkbox compliance to evidence-based lifecycle control.
Where independent technical benchmarking adds value
One challenge in healthcare procurement and maintenance planning is that supplier claims do not always reflect field reality. Devices may meet minimum compliance requirements while still differing substantially in durability, signal quality, service access, or long-term reliability. This is where independent benchmarking and engineering-focused assessment become valuable.
An evidence-based review process can help decision-makers compare not just whether equipment is certified, but whether it is maintainable, supportable, and operationally resilient. For organizations evaluating equipment across Surgical & Clinical Tech, Laboratory & Life Sciences, and Rehabilitation & Bionics, this kind of technical scrutiny reduces uncertainty before maintenance burdens become expensive operational problems.
For example, comparing factors such as material fatigue limits, sensor stability, environmental tolerance, service documentation quality, and performance consistency can materially improve both procurement outcomes and maintenance forecasting.
Conclusion
Hospital equipment standards affect maintenance planning far beyond basic compliance. They shape service intervals, testing requirements, staff responsibilities, documentation quality, software control, and replacement timing. For operators, procurement teams, and healthcare leaders, the real priority is to translate standards into practical maintenance decisions that protect uptime, patient safety, and lifecycle value.
The strongest approach is to evaluate equipment not only for purchase readiness, but for maintainability across its full operational life. When hospitals align maintenance planning with hospital equipment standards, MDR certification expectations, and disciplined medical device assessment, they make better sourcing decisions, reduce operational risk, and build a more reliable healthcare technology environment.
- EMS
- ESS
- PPE
- healthcare technology
- life sciences
- procurement
- cybersecurity
- AR
- Cement
- material fatigue
- benchmarking
- healthcare procurement
- MDR certification
- value-based procurement
- hospital equipment standards
- medical device assessment
- regulatory compliance
- technical benchmarking
- material fatigue
- life sciences
- long-term reliability
- clinical performance
- healthcare technology
Recommended News
- 2026.04.23Low-Altitude Economy Enters Scale-Up Year: eVTOL Infrastructure & Vital Sign SensingLydia Vancini (Regulatory Compliance Lead)
- 2026.04.23Lianyirong, ABC Shanghai Dongfang Hub Branch Close Two e-NI TransactionsDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.04.23China’s April 2026 LPR Set at 3.0% (1Y) and 3.5% (5Y+): Implications for Medical Device Export Financing
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
