How to plan healthcare equipment sourcing for 2026?
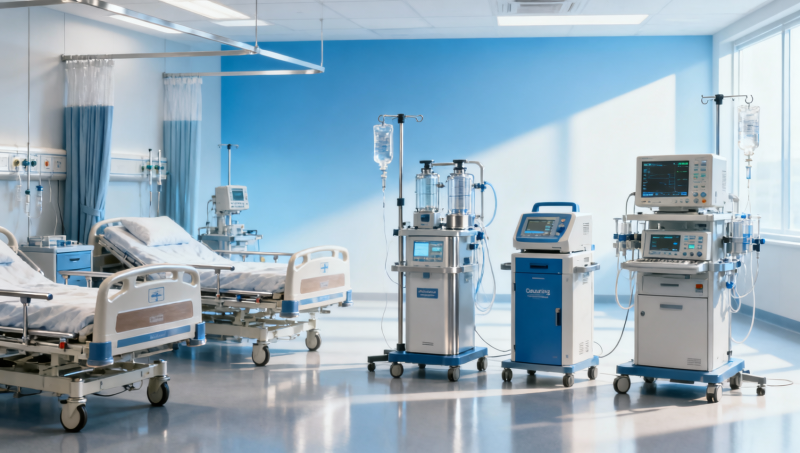
Planning healthcare equipment sourcing for 2026 means going beyond price lists and product claims. From hospital furniture wholesale and oxygen concentrator factory selection to IVDR certification, supply chain verification, and digital integration, buyers need evidence-based decisions. This guide helps procurement teams, operators, and healthcare leaders evaluate healthcare equipment with a healthcare engineering mindset—reducing risk, improving compliance, and sourcing with greater confidence.
For hospitals, laboratories, outpatient networks, and MedTech project teams, the 2026 sourcing cycle will be shaped by three realities: tighter compliance expectations, more complex connected devices, and greater scrutiny over total cost of ownership across 3–7 years. The practical question is no longer whether a supplier can ship equipment. It is whether that supplier can prove repeatable performance, documented quality controls, and stable after-sales support under real operating conditions.
That is where a technical benchmarking approach becomes valuable. VitalSync Metrics (VSM) focuses on converting manufacturing variables, validation logic, and performance thresholds into structured decision inputs. For information researchers, operators, procurement managers, and business decision-makers, a better sourcing plan starts with measurable criteria, not sales language.
Define the 2026 sourcing scope before requesting quotations
A common procurement mistake is sending RFQs too early. In healthcare equipment sourcing, this often leads to mismatched specifications, hidden accessories, and unrealistic delivery assumptions. Before comparing suppliers, teams should define the sourcing scope across 4 layers: clinical use, operational workflow, regulatory class, and digital integration needs. This reduces rework during evaluation and shortens approval cycles by 2–4 weeks.
For example, hospital furniture wholesale decisions should not be grouped under the same logic as oxygen concentrator factory selection. A bed, cabinet, or treatment trolley is evaluated around load range, corrosion resistance, cleanability, and mobility. An oxygen concentrator requires a different evidence set: flow stability, alarm logic, power tolerance, maintenance interval, and spare-parts continuity. Grouping unlike products under one purchasing template creates avoidable risk.
In 2026, sourcing plans should also separate capital equipment from high-turnover support devices. Capital equipment may require a 5–10 year service view, while support devices may be reviewed on 12–24 month performance cycles. This distinction affects warranty expectations, vendor audits, inventory planning, and budget approvals.
Build a sourcing brief around operational reality
A strong sourcing brief should capture actual workflow conditions, not ideal laboratory assumptions. Include room temperature range, typical operating hours per day, operator skill level, cleaning agents used on-site, power stability, and network environment. A device that performs well in a controlled demo may underperform when used 16 hours per day in a crowded ward or laboratory.
Core elements to define before supplier outreach
- Clinical application and user group, such as ICU, outpatient, home care, diagnostics, or sterile processing.
- Expected duty cycle, for example 8, 12, or 24 hours per day, and anticipated annual utilization volume.
- Required compliance pathway, including MDR, IVDR, electrical safety, sterilization compatibility, or biocompatibility evidence where relevant.
- Facility constraints such as door clearance, floor load, gas supply, voltage range, and data interface requirements.
- Service expectations, including response time within 24–72 hours, spare-parts lead time, and preventive maintenance frequency.
The table below shows how healthcare buyers can segment equipment categories before issuing tenders. This type of early classification helps procurement, operators, and management align on technical depth, risk profile, and review effort.
The key takeaway is simple: a sourcing plan becomes more reliable when the equipment portfolio is segmented early. It prevents under-specification in critical devices and over-engineering in low-risk categories, which can improve tender clarity and supplier comparability from the beginning.
Evaluate suppliers by technical evidence, not marketing language
By 2026, procurement teams will face an even wider gap between promotional claims and verified healthcare equipment performance. A polished brochure may mention efficiency, safety, and smart integration, but these are not decision-grade inputs. Buyers need evidence that can be checked: test methods, production controls, tolerance ranges, failure modes, and post-market service logic.
This matters especially when selecting an oxygen concentrator factory, a laboratory device manufacturer, or a supplier of connected monitoring systems. Ask whether the supplier can show performance consistency across batches, not just a single sample. Ask how often calibration drift is checked. Ask which components are single-sourced and which are dual-sourced. These questions often reveal more than price ever will.
For procurement teams, a practical way to compare healthcare equipment suppliers is to use a weighted evidence matrix. This method supports both commercial review and technical review, especially when multiple departments must approve a purchase within a 30–90 day decision window.
What technical evidence should be requested?
The evidence package should match the product category, but most sourcing projects should request manufacturing consistency records, quality control checkpoints, maintenance manuals, cleaning validation information, and proof of service capability. For connected devices, add cybersecurity update logic, interoperability notes, and software version control records.
A practical 5-point supplier review checklist
- Can the supplier explain the key performance threshold in measurable terms, such as output variation, sensor accuracy, or load endurance?
- Can they provide routine inspection or batch-level verification records from the last 6–12 months?
- Do they document expected service intervals, spare-parts replacement cycles, and field failure response procedures?
- Can they support your market with compliant documentation for MDR, IVDR, or equivalent jurisdictional requirements?
- Do they have a realistic logistics and support model for installation, training, and technical escalation?
The following comparison table can be used during technical screening. It helps teams move from generic impressions to measurable sourcing criteria.
When buyers use evidence-based comparison, weak claims become easier to filter out. That is especially useful in global sourcing, where differences in documentation quality, factory maturity, and after-sales structure can be substantial even when quoted prices appear similar.
Plan for compliance, IVDR/MDR readiness, and traceability
Healthcare equipment sourcing for 2026 must account for regulatory alignment much earlier in the process. In Europe and other tightly regulated markets, MDR and IVDR are no longer checklist topics left for the end of procurement. They affect product selection, supplier qualification, documentation review, import timing, and go-live schedules.
Even when a buyer is not directly importing into the EU, MDR and IVDR principles still influence sourcing decisions because they push suppliers toward stronger traceability, risk management, and technical documentation practices. For laboratory architects and diagnostics stakeholders, IVDR readiness is especially relevant when assessing instruments, accessories, and data-handling workflows that support in vitro testing environments.
From an operational standpoint, traceability must extend beyond certificates. Procurement teams should confirm the document version control process, serial or batch traceability logic, complaint handling path, and change notification protocol. A supplier that changes a critical component without clear notification can create validation, compatibility, or maintenance issues months after installation.
Compliance questions to ask before awarding a contract
At minimum, buyers should ask how documentation is maintained, how nonconformities are managed, and how design or component changes are communicated. For higher-risk equipment, also ask about risk files, labeling controls, cleaning instructions, and user training materials. If software is involved, request information on release control and cybersecurity update handling over a period of at least 24 months.
Common compliance gaps that delay healthcare equipment projects
- Documentation exists, but the latest revision is not clearly identified or linked to shipped batches.
- Import and distributor responsibilities are not defined, creating delays during customs or local registration review.
- Cleaning, disinfection, or reprocessing instructions are too generic for actual hospital use.
- Labels, IFUs, or language versions are incomplete for the target market.
- Software-connected systems lack a documented change control path, increasing cybersecurity and validation risk.
The table below highlights how compliance planning can be integrated into sourcing timelines instead of being treated as a final-stage administrative task.
Treating compliance as an integrated sourcing workstream reduces downstream disruption. It also helps decision-makers compare suppliers on readiness, not just on product availability. In many cases, that leads to fewer launch delays and a cleaner acceptance process after delivery.
Manage total cost, delivery risk, and digital integration together
In healthcare procurement, a lower purchase price can still produce a higher total cost over 3–5 years. This happens when maintenance is frequent, consumables are proprietary, spare parts take 6–8 weeks to arrive, or devices cannot connect reliably to existing digital systems. For 2026 sourcing plans, cost, logistics, and interoperability should be reviewed as one combined risk area.
Digital integration is now relevant across a wide equipment range. Bedside monitors, oxygen systems, laboratory analyzers, and even some hospital furniture platforms may require connectivity for asset tracking, usage monitoring, or workflow coordination. If interfaces, protocols, or cybersecurity responsibilities are undefined during procurement, the equipment may remain underused after installation.
Procurement teams should therefore model total landed value rather than unit price alone. Include shipping mode, import costs, installation support, training effort, spare-parts stocking, calibration needs, downtime risk, and software update dependencies. In many healthcare settings, a device with a 10% higher purchase price but 30% lower service burden can be the better decision.
A practical implementation flow for 2026 sourcing projects
- Map equipment categories and rank them by clinical criticality, utilization level, and compliance impact.
- Define technical and operational requirements with end users, biomedical teams, IT, and procurement.
- Run supplier pre-screening based on documentation quality, service reach, and manufacturing transparency.
- Compare shortlisted suppliers using weighted scoring for technical evidence, cost, lead time, and integration readiness.
- Confirm acceptance testing, training, spare-parts planning, and change control terms before final award.
Typical risk controls to include in the contract
Contracts should specify delivery windows, installation responsibilities, response times, replacement logic for defective units, and component change notification. For connected equipment, include software support duration and responsibilities for interface adjustments. For multisite deployments, it is also useful to set phased acceptance milestones, such as pilot, site validation, and full rollout within 60–120 days.
A sourcing plan built this way supports operators as well as finance leaders. Operators get equipment that fits workflow and maintenance reality. Procurement gets cleaner supplier comparison. Executives get better visibility into long-term risk and capital efficiency. That combination is what makes healthcare equipment sourcing more resilient in 2026.
FAQ for procurement teams, operators, and healthcare decision-makers
How early should healthcare equipment sourcing for 2026 begin?
For standard equipment, many organizations should begin 4–6 months before the target deployment date. For regulated or digitally integrated systems, 6–9 months is more realistic. This allows time for technical review, compliance checks, budget approvals, logistics planning, and installation readiness without compressing critical validation steps.
What should buyers focus on when selecting an oxygen concentrator factory?
Focus on output stability, maintenance interval, alarm system logic, spare-parts availability, and production consistency. Ask how performance is verified across batches, not just at prototype level. Also confirm service documentation, power tolerance, and the expected lead time for replacement components, which is often a hidden risk in respiratory device sourcing.
Why is hospital furniture wholesale still a technical sourcing issue?
Because furniture in healthcare settings affects infection control, staff ergonomics, patient safety, and lifecycle cost. Buyers should review load capacity, caster quality, surface resistance to cleaning agents, weld consistency, and maintenance requirements. In high-turnover environments, small specification errors can multiply across 50, 100, or 300 units.
How can VSM support a more reliable sourcing process?
VSM brings an engineering-led perspective to healthcare equipment selection by translating technical variables into decision-ready comparisons. Instead of relying on promotional claims alone, buyers can assess measurable performance, documentation maturity, compliance alignment, and long-term reliability. This is especially useful for teams managing cross-border sourcing, regulated categories, or complex equipment portfolios.
A successful 2026 sourcing plan is built on structured requirements, technical evidence, compliance readiness, and a clear view of lifecycle risk. Whether the project involves hospital furniture wholesale, oxygen concentrator factory assessment, IVD-related documentation review, or digital integration planning, the same principle applies: procurement performs better when engineering truth is easier to see.
VitalSync Metrics (VSM) helps healthcare buyers cut through noise with data-driven benchmarking and practical sourcing insight. If your team needs a more defensible way to compare suppliers, verify healthcare equipment performance, or prepare a customized 2026 procurement roadmap, contact us to discuss your application, request a tailored evaluation framework, or explore more healthcare sourcing solutions.
- global sourcing
- EMS
- ESS
- hospital furniture
- PPE
- EdTech
- procurement
- cybersecurity
- AR
- supply chain
- Cement
- benchmarking
- healthcare procurement
- technical benchmarking
- digital integration
- supply chain
- long-term reliability
- engineering truth
- data-driven
- healthcare engineering
- IVDR certification
- healthcare equipment
- supply chain verification
- oxygen concentrator factory
- hospital furniture wholesale
Recommended News
- 2026.04.17Hospital equipment standards shaping modern rehab devicesSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.04.17Laboratory equipment validation errors in sample storageDr. Hideo Tanaka (Imaging Systems Analyst)
- 2026.04.17Medical equipment certification delays in remote monitoringLydia Vancini (Regulatory Compliance Lead)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
