Ultrasound transducer frequency range and image depth tradeoffs
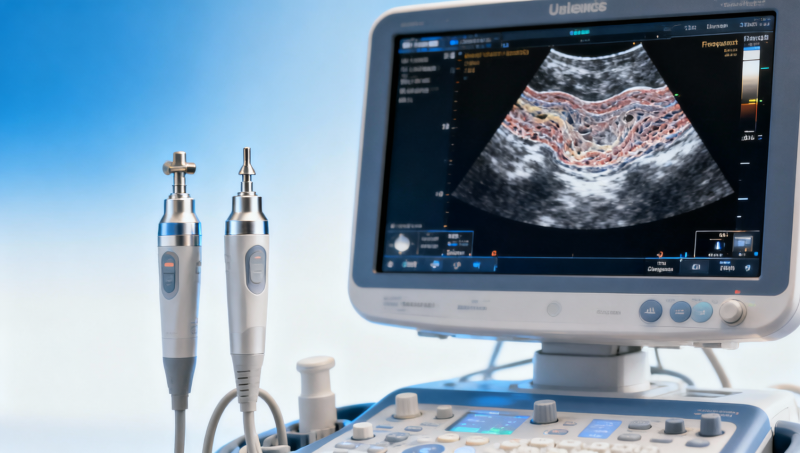
Choosing the right ultrasound transducer frequency range is always a tradeoff between image detail and penetration depth. For clinicians, buyers, and MedTech evaluators, understanding this balance is as critical as reviewing signal to noise ratio in patient monitors or meeting biocompatibility testing standards. This guide explains how frequency affects diagnostic performance, helping you assess technical claims, compare device specifications, and make more confident procurement decisions.
In practical terms, the frequency range of an ultrasound transducer shapes what can be seen, how clearly it can be seen, and in which patient population it can be used reliably. A 3–5 MHz convex probe and a 10–18 MHz linear probe may both appear in the same product catalog, yet they serve very different clinical and procurement purposes. For operators, the issue is image usability at the bedside. For purchasing teams, the issue is whether stated specifications translate into repeatable diagnostic performance across departments and patient types.
For healthcare organizations moving toward value-based procurement, frequency selection is not a narrow technical choice. It affects exam workflow, training burden, replacement planning, multi-department standardization, and long-term equipment utilization. That is why frequency range should be evaluated alongside footprint, bandwidth, acoustic output, compatibility, serviceability, and documentation quality rather than as a single line item on a quotation sheet.
How Ultrasound Frequency Range Influences Image Formation
Ultrasound transducer frequency refers to the number of sound wave cycles emitted per second, typically expressed in megahertz. In diagnostic systems, common ranges span from about 2 MHz to 18 MHz, while specialty applications may go lower or higher. Lower frequencies penetrate deeper into tissue, but they produce less spatial detail. Higher frequencies generate sharper resolution, yet their energy attenuates more quickly and therefore cannot reach deeper targets as effectively.
This tradeoff matters because attenuation increases with frequency. As sound travels through tissue, part of the wave is absorbed or scattered. If attenuation is too high before the beam reaches the area of interest, the returning echoes become weak and the final image loses diagnostic value. That is why abdominal imaging often relies on lower-frequency probes in the 2–5 MHz range, whereas superficial vascular or musculoskeletal imaging commonly uses 7–15 MHz or higher.
Resolution also has multiple dimensions. Axial resolution improves with shorter pulse length, which generally benefits from higher frequency. Lateral resolution depends on beam focusing, aperture, and system design, not frequency alone. For procurement teams, this means a broad stated bandwidth is useful, but it should not be mistaken for guaranteed performance without supporting evidence such as phantom testing, depth-specific uniformity, and grayscale contrast response.
Why the Same Probe Specification Can Perform Differently
Two probes labeled 5–12 MHz may not deliver the same image quality. Piezoelectric material, matching layers, backing design, cable shielding, beamforming electronics, and software processing all influence performance. A nominal range in a brochure may describe tunable operating bandwidth, but the clinically useful range can be narrower in real scanning conditions.
This is especially important when comparing handheld devices, cart-based systems, and OEM-supplied probes. Handheld platforms may use advanced reconstruction software to compensate for size and power constraints, while premium console systems may preserve better penetration at mid-band frequencies. Buyers should therefore ask not only “What is the frequency range?” but also “At what depth and under what preset does this range achieve usable contrast and border definition?”
Core technical checkpoints
- Identify the center frequency and usable bandwidth, not just the maximum advertised frequency.
- Review image depth performance at 4 cm, 8 cm, 12 cm, and 20 cm where applicable.
- Check whether harmonics, compound imaging, and beam steering alter practical penetration.
- Confirm compatibility between transducer type and the intended clinical preset library.
The table below summarizes the relationship between ultrasound transducer frequency range and depth expectations across common clinical scenarios. These values are general planning ranges rather than universal guarantees, because patient body habitus and system architecture can shift actual results.
For most procurement decisions, the key conclusion is simple: no single ultrasound transducer frequency range is ideal for every department. Facilities seeking one-probe versatility often compromise image detail, while facilities that match frequency to task usually achieve better diagnostic confidence and fewer operator complaints.
Matching Frequency Range to Clinical Application and User Needs
The right probe is determined by anatomy depth, patient variability, and workflow purpose. Emergency medicine may prioritize speed and adequate penetration across mixed body types. Vascular labs may prioritize wall detail, plaque characterization, and needle visualization at shallow depths. Surgical teams may need compact footprints and sterile workflow compatibility. In each case, ultrasound transducer frequency range should be interpreted through the lens of the exam target rather than marketing hierarchy.
For operators, a frequent mistake is selecting the highest available frequency because the image appears sharper on a thin patient or phantom. In real practice, edema, obesity, dressings, or deeper targets can reduce usefulness. A probe that performs well at 3 cm but degrades rapidly beyond 5 cm may not support consistent bedside decisions. Clinical usability depends on whether the transducer maintains acceptable contrast, edge definition, and Doppler sensitivity within the actual scanning depth required.
For procurement teams, application mapping should include at least 4 dimensions: department, anatomy depth, patient population, and operator skill level. A tertiary hospital may justify multiple specialized probes, while an outpatient center may prefer two versatile transducers covering 80%–90% of routine exams. Decision-makers should also consider training time. Transitioning staff to a new probe family can require 2–6 weeks of supervised adaptation depending on interface changes and preset behavior.
Typical application-fit considerations
- Deep abdominal and obstetric assessments usually favor lower frequencies for 15–25 cm penetration.
- Peripheral vascular work often benefits from 7–12 MHz to resolve superficial vessel walls and needle tips.
- Musculoskeletal and nerve imaging commonly requires 10–18 MHz for tendons, ligaments, and small structures.
- General point-of-care ultrasound often works best with a balanced range that preserves flexibility over maximum detail.
The following comparison table can help stakeholders map application priorities to realistic transducer choices rather than relying on a single specification line.
The practical takeaway is that application fit should be judged by the percentage of target exams covered without clinically meaningful compromise. If a transducer supports only 50%–60% of routine workflows well, the apparent price advantage may disappear through repeat scans, added accessories, and operator dissatisfaction.
What Buyers Should Verify Beyond the Frequency Number
A procurement-grade evaluation should go beyond catalog claims. The stated ultrasound transducer frequency range is only one part of a broader technical and operational profile. Decision-makers should verify at least 6 areas: usable imaging depth, spatial resolution, cable and connector durability, cleaning and disinfection compatibility, preset flexibility, and service response terms. In high-utilization environments, even small weaknesses can create measurable downtime within 12–24 months.
Another critical issue is test methodology. Some vendors showcase excellent superficial detail using optimized phantoms or ideal patients, yet the probe may underperform in heavier body habitus or at deeper focal zones. For this reason, comparative validation should include a standardized phantom review and, where policy allows, controlled user evaluation under routine settings. It is often useful to compare image quality at fixed depths such as 4 cm, 8 cm, and 12 cm rather than relying on subjective impressions alone.
Regulatory and lifecycle factors also matter. Hospital buyers increasingly assess whether supplied documentation supports device traceability, maintenance planning, and region-specific compliance obligations. While transducer frequency itself does not determine MDR or IVDR relevance, the surrounding technical file, performance consistency, labeling clarity, and service documentation influence overall procurement confidence. The more complex the platform, the more important independent benchmarking becomes.
A practical 5-step evaluation workflow
- Define the top 3–5 exam types that drive purchase justification.
- Set minimum acceptable depth and detail targets for each use case.
- Request side-by-side scans or phantom evidence under matched settings.
- Review warranty, repair turnaround, and replacement loaner policy, ideally within 5–10 business days.
- Calculate total cost over 3 years, including accessories, service events, and training time.
Common evaluation blind spots
One recurring blind spot is assuming that broader bandwidth automatically means better clinical coverage. Another is ignoring ergonomics. A technically capable probe that causes hand fatigue during a 20-minute vascular exam may reduce user acceptance. Buyers should also inspect strain relief points, connector wear resistance, and reprocessing instructions, because these factors strongly affect failure rates in high-turnover departments.
At organizations like VitalSync Metrics, the value of benchmarking lies in translating engineering parameters into procurement clarity. When technical claims are compared against standardized review criteria, teams can separate true performance advantages from surface-level specification inflation. This approach supports better vendor conversations and reduces risk in tenders where multiple products appear similar on paper.
Balancing Image Depth, Resolution, Cost, and Standardization
The best transducer strategy is rarely about maximizing one attribute. It is about balancing image depth, detail, capital efficiency, and operational consistency. For a multi-site provider, standardizing around 2 or 3 transducer categories may reduce training complexity and spare-part inventory. For a specialty center, however, deeper specialization may create better clinical value even if the unit price is higher. The right decision depends on case mix, utilization rate, and staffing model.
Cost should be analyzed across the full lifecycle. A lower-priced probe with narrower useful bandwidth may lead to duplicate purchases, more frequent replacements, or reduced exam confidence. Conversely, an advanced high-frequency probe may offer exceptional detail but remain underused if only a small fraction of patients require that performance. In many settings, the most efficient portfolio is one that covers 70%–80% of routine exams with standard probes and reserves specialty probes for defined indications.
Standardization can also improve data quality across departments. When imaging teams use consistent probe families and preset logic, image interpretation becomes more predictable and training becomes easier to scale. This matters in networks with rotating staff, satellite clinics, or centralized procurement. The objective is not uniformity for its own sake, but a controlled balance between flexibility and reliability.
Decision factors by stakeholder group
This table shows that a “best probe” does not exist in isolation. The optimal ultrasound transducer frequency range must fit a decision context. A superficial imaging clinic may prioritize frequency-driven detail, while a network procurement office may prioritize fleet consistency and service performance over peak specification values.
Common Misconceptions, Risk Points, and Selection Questions
One common misconception is that higher frequency always means better imaging. In reality, better imaging means fit-for-purpose imaging. A 15 MHz probe can outperform a 5 MHz probe for tendon structure at 2 cm, yet fail to visualize a deep abdominal target at 18 cm. Another misconception is that software enhancements can fully replace acoustic limitations. Signal processing can improve display quality, but it cannot fully restore information that never returned from depth.
There are also operational risks. If departments choose probes independently without a shared evaluation framework, organizations may end up with overlapping frequency ranges but inconsistent connectors, accessories, and cleaning workflows. This complicates training and raises maintenance overhead. A more disciplined approach is to build a selection matrix with 4 categories: performance, usability, compliance, and support.
For buyers comparing vendors, the most useful questions are often very specific. Ask what proportion of image quality claims are based on harmonic imaging. Ask whether the quoted frequency range reflects default presets or full manual tuning. Ask how performance changes after repeated disinfection cycles. Ask whether replacement turnaround is measured in calendar days or business days. These details influence operational reality more than headline marketing phrases.
FAQ for clinical and procurement teams
How do I choose an ultrasound transducer frequency range for mixed-use departments?
Start by identifying the top 5 exam categories and their typical depth ranges. If most studies fall between superficial vascular access and routine abdominal screening, a dual-probe strategy often works better than one universal probe. In many mixed environments, pairing a 2–5 MHz convex or phased option with a 7–12 MHz linear option covers the majority of cases more reliably than forcing a single mid-band probe to handle every task.
What frequency range is best for deeper patients?
For deeper penetration, lower frequencies such as 2–5 MHz are usually more effective because attenuation is reduced. However, lower frequency alone is not enough. Beamforming quality, output power management, focusing behavior, and system noise control all influence whether deep structures remain interpretable at 15–25 cm.
Should procurement teams accept brochure specifications at face value?
No. Brochure values are useful for screening but not sufficient for selection. Procurement teams should request demonstration evidence, comparable test conditions, service documentation, and practical imaging examples at defined depths. A structured review during a 2–4 week evaluation period often reveals usability and consistency issues that are invisible in static specification sheets.
How often do transducer-related issues affect long-term ownership cost?
In high-use environments, cable wear, strain relief fatigue, connector issues, and reprocessing damage can affect ownership cost as much as image performance. That is why lifecycle planning should include inspection intervals, cleaning compatibility, and expected service response. Even one probe replacement event can significantly change the effective cost of a low-priced purchase.
Selecting the right ultrasound transducer frequency range is ultimately a question of evidence-based fit. Frequency determines the balance between image detail and penetration depth, but real procurement value comes from understanding how that balance performs in actual workflows, patient populations, and maintenance conditions. For information researchers, operators, procurement teams, and enterprise leaders, a disciplined comparison framework reduces technical ambiguity and supports more reliable purchasing decisions.
VitalSync Metrics supports this decision process by translating engineering performance into procurement-ready insight. If you need help benchmarking ultrasound specifications, comparing suppliers, or building a more defensible selection matrix for healthcare technology purchasing, contact us to discuss your use case, request a tailored evaluation approach, or explore more MedTech verification solutions.
Recommended News
- 2026.06.02Smart Street Lighting Cost-Effective Solutions: Controls, LEDs, and ROILydia Vancini (Regulatory Compliance Lead)
- 2026.06.02Stepper Motors Selection Guide: Torque, Step Angle, Drivers, and Load FitDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.06.02UV Water Sterilizers for Small Facilities: Flow Rate, Dose, and Lamp LifeDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
