Endoscope image resolution benchmark: where specs stop matching reality
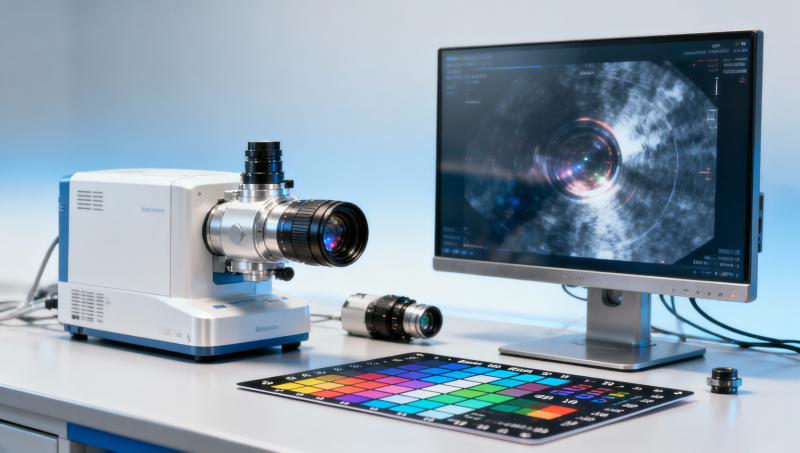
On paper, an endoscope image resolution benchmark looks simple: compare pixel counts and published specs. In reality, clinical image quality is shaped by optics, illumination, signal processing, and the signal to noise ratio in patient monitors and adjacent medical electronics workflows. This article examines where datasheets fail, why benchmark methods matter, and how buyers and technical teams can verify performance beyond marketing claims.
For hospital procurement teams, operating room users, MedTech founders, and technical evaluators, the gap between brochure language and usable image quality can directly affect adoption risk, training burden, and total cost of ownership. A 4K label, for example, does not guarantee accurate tissue edge rendering, stable color reproduction, or low-noise visualization in narrow lumens.
That is why an endoscope image resolution benchmark should be treated as a systems evaluation, not a single-number comparison. Resolution interacts with lens quality, illumination uniformity, sensor behavior, compression, display chain integrity, and even electromagnetic conditions in connected clinical environments. Independent benchmarking helps convert these variables into procurement-grade evidence.
Why datasheet resolution rarely predicts clinical image performance
An endoscope image resolution benchmark often starts with a familiar claim: 1080p, 2K, or 4K output. Yet a clinical image is not created by output pixels alone. The visible result depends on at least 5 linked stages: lens capture, sensor conversion, signal processing, transport, and display rendering. Weakness at any stage reduces effective detail, even if the final video stream still reports a high pixel format.
Optical performance is one of the most common blind spots. Two systems may both advertise 3840 × 2160 output, but if one uses lower-grade optics with edge softness, chromatic aberration, or poor illumination coupling, the user may perceive less usable detail at the distal end. In practical workflows, effective resolution can drop by 15%–30% from center to edge of field.
Signal processing is another hidden variable. Aggressive sharpening can make a still image look crisp during a demo, but it may also introduce halos and false tissue boundaries. Noise reduction can smooth the picture, yet remove microtexture that operators rely on for orientation. When benchmark methods ignore processing artifacts, buyers may approve a system that performs well in showroom conditions but inconsistently in real procedures.
Clinical image quality also depends on stability over time. A system that performs well for 10 minutes may drift after 45–60 minutes due to heat, illumination shift, or processor throttling. For laboratories and procurement committees, this means acceptance testing should include sustained-use evaluation, not just a single short capture sequence.
Common reasons published specs stop matching reality
- Output resolution is listed, but optical resolving power at the distal tip is not measured.
- Bench photos are taken under ideal lighting instead of low-light or high-reflection scenarios common in procedures.
- Compression behavior is not disclosed, especially in recording or networked viewing workflows.
- Display chain variables, including monitor scaling and monitor signal-to-noise behavior, are excluded from evaluation.
- Manufacturers report peak performance, while users need average and worst-case behavior across 3–4 procedural conditions.
The table below shows why an endoscope image resolution benchmark should separate “declared specifications” from “clinically usable image factors.” This distinction is especially important in value-based procurement, where technical evidence must support lifecycle decisions rather than one-time demonstrations.
The key lesson is simple: a higher listed resolution may improve capability, but it does not by itself confirm diagnostic usability or workflow reliability. A credible benchmark translates technical layers into repeatable evidence that procurement teams, operators, and executive stakeholders can compare on equal terms.
What a rigorous benchmark should actually measure
A meaningful endoscope image resolution benchmark must go beyond one chart image and one monitor. At minimum, it should test optical resolution, illumination uniformity, signal-to-noise performance, color consistency, geometric distortion, latency, and repeatability. In practical terms, that means at least 6–8 test dimensions rather than a single “line pairs” result.
Test conditions matter as much as metrics. Benchmarking should include 3 common viewing scenarios: standard target distance, near-field close-up, and low-light or reflective conditions. If a device only performs well at one fixed working distance, the reported resolution may overstate real performance in anatomy with variable depth and surface reflectance.
Display chain validation is equally important. A strong imaging head connected to a noisy processor, a mismatched monitor, or unstable adjacent electronics can reduce perceived clarity. In integrated operating rooms and digital labs, electromagnetic and power quality conditions may slightly elevate image noise, especially when multiple devices operate simultaneously within the same workflow stack.
Benchmark repeatability should also be defined in advance. For procurement-grade testing, repeating each key measurement 3 times across separate sessions is a practical baseline. If measured center resolution or color deviation varies widely between sessions, the issue may be manufacturing variance, thermal drift, or poorly controlled processing behavior.
Core benchmark dimensions
Technical metrics that deserve procurement attention
- Optical resolving power at center and edge of field, ideally measured at 2 or more working distances.
- Illumination uniformity, because bright center and dim edges can erase practical visibility.
- Signal-to-noise ratio under normal and low-light conditions, not just in ideal exposure.
- Color fidelity and white balance stability across 20–30 minutes of continuous operation.
- Latency and frame stability, particularly if the image is routed through recording, networking, or processing modules.
The following table outlines a practical framework that engineering teams and purchasing committees can use when defining an endoscope image resolution benchmark for vendor comparison, incoming inspection, or independent laboratory review.
When these metrics are standardized, benchmark results become far more useful than isolated vendor demos. They enable side-by-side comparison, support evidence files for procurement reviews, and reduce disputes after installation when user expectations meet everyday clinical workflow.
How buyers, users, and technical teams should evaluate systems before purchase
Different stakeholders look at the same system through different risk lenses. Operators care about visibility, handling confidence, and consistency. Procurement teams focus on comparability, service burden, and lifecycle value. Business leaders want lower adoption risk and clearer evidence that the selected platform will remain viable across 3–5 years of use and digital integration.
A smart pre-purchase evaluation uses a layered workflow. First, review published technical documentation and identify missing parameters. Second, define acceptance criteria for 4–6 measurable items such as edge sharpness, low-light noise, white balance stability, and compatibility with existing monitors or recording systems. Third, run side-by-side testing in a controlled environment before pilot deployment.
It is also useful to separate “demo quality” from “workflow quality.” Many systems are optimized for short demonstrations on carefully calibrated displays. Actual use may involve shared displays, routing through video processors, image capture software, or adjacent patient monitoring infrastructure. These conditions can expose weaknesses that do not appear during a 15-minute sales session.
For MedTech startups and laboratory architects, independent benchmark documentation can also support design validation and supplier qualification. Instead of accepting a supplier’s top-line output claim, teams can request benchmark evidence tied to use cases, repeatability, and tolerance bands. That shortens qualification cycles and reduces redesign risk later in the program.
A practical pre-procurement checklist
- Confirm whether stated resolution refers to sensor pixels, processed output, or displayed monitor format.
- Request image samples captured at more than 1 distance and under at least 2 illumination conditions.
- Verify compatibility with current display, recording, and digital archiving systems.
- Ask whether image processing modes can be locked, documented, and reproduced across units.
- Include a sustained-use test of 30–60 minutes to detect heat-related drift or instability.
- Document acceptance thresholds before comparison to avoid subjective decision-making.
Decision criteria that matter more than brochure claims
In many procurement settings, the winning system is not the one with the highest nominal resolution. It is the one that maintains image consistency across users, rooms, displays, and time. If two products are close in price but one reduces reconfiguration steps, user complaints, or service calls over a 24-month period, its operational value may be higher even without a headline spec advantage.
This is where an independent technical benchmark adds business value. It turns subjective impressions into measurable decision factors and helps stakeholders align around a common evidence base. That is especially important in healthcare procurement, where clinical utility, compliance expectations, and digital interoperability increasingly converge.
Implementation risks, common mistakes, and how to reduce post-purchase disappointment
One of the biggest mistakes in endoscope image resolution benchmark projects is testing too narrowly. A procurement team may approve a system based on one chart, one display, and one operator. But real deployment introduces 4 common stressors: different users, longer procedures, variable anatomy, and integration with other electronics. If these stressors are ignored, post-purchase complaints often appear within the first 30–90 days.
Another common mistake is failing to control the test environment. Ambient light, monitor calibration, cable quality, processor settings, and power conditions can all influence results. When comparison protocols are not standardized, a weaker system can appear competitive simply because it was demonstrated under more favorable conditions.
There is also a documentation gap in many buying processes. Teams capture screenshots and subjective notes, but do not record firmware version, processing mode, working distance, illumination level, or routing path. Without those details, later troubleshooting becomes difficult, and supplier discussions can turn into opinion rather than evidence.
Independent benchmarking laboratories reduce this uncertainty by applying repeatable protocols, controlled setups, and standardized reporting. For organizations pursuing stronger technical due diligence, this supports supplier qualification, incoming verification, and more defensible capital equipment decisions.
Typical risk areas and mitigation actions
The matrix below highlights where specification-driven buying frequently fails, and what a more disciplined verification process should include before final approval or rollout.
The practical conclusion is that technical integrity must be validated as a system property. Resolution is important, but procurement outcomes improve when teams benchmark the full image pathway and document findings in a structured format that can survive internal review, supplier negotiation, and future audit needs.
FAQ for procurement and technical review
How many units should be tested before a decision?
For high-value procurement, testing at least 2 units or 2 sample configurations is a sensible minimum when feasible. This helps detect unit-to-unit variance, especially if the system includes adjustable processing profiles or interchangeable display components.
Is 4K always better than 1080p in endoscope imaging?
Not always. If optics, illumination, and noise behavior are weak, a 4K pipeline may not deliver meaningfully better usable detail than a strong 1080p system. Benchmarking should focus on effective detail, low-light retention, and image stability rather than pixel format alone.
How long does a meaningful benchmark process usually take?
A focused lab evaluation can often be organized in 7–15 business days once samples, protocols, and acceptance criteria are defined. More complex projects involving integration review, multi-scenario testing, or comparative reporting may extend to 2–4 weeks.
Which teams benefit most from independent benchmark reports?
Procurement directors, clinical engineering teams, laboratory planners, MedTech product managers, and executive decision-makers all benefit. Each group gains a different advantage: less ambiguity, better comparability, clearer risk visibility, and stronger confidence in capital or supplier decisions.
An endoscope image resolution benchmark becomes valuable when it reveals what specifications hide: the difference between advertised output and dependable clinical performance. For healthcare organizations and MedTech teams navigating value-based procurement, that difference affects usability, compliance readiness, supplier trust, and long-term lifecycle cost.
VitalSync Metrics (VSM) supports this need with independent, data-driven benchmarking that turns complex technical variables into standardized, decision-ready evidence. If you need to compare systems, validate supplier claims, or build a more defensible procurement process, contact VSM to discuss a tailored benchmark plan, request technical evaluation support, or learn more about healthcare engineering verification solutions.
Recommended News
- 2026.06.02Smart Street Lighting Cost-Effective Solutions: Controls, LEDs, and ROILydia Vancini (Regulatory Compliance Lead)
- 2026.06.02Stepper Motors Selection Guide: Torque, Step Angle, Drivers, and Load FitDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.06.02UV Water Sterilizers for Small Facilities: Flow Rate, Dose, and Lamp LifeDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
