Healthcare Analytics Metrics That Support Smarter Budget Calls
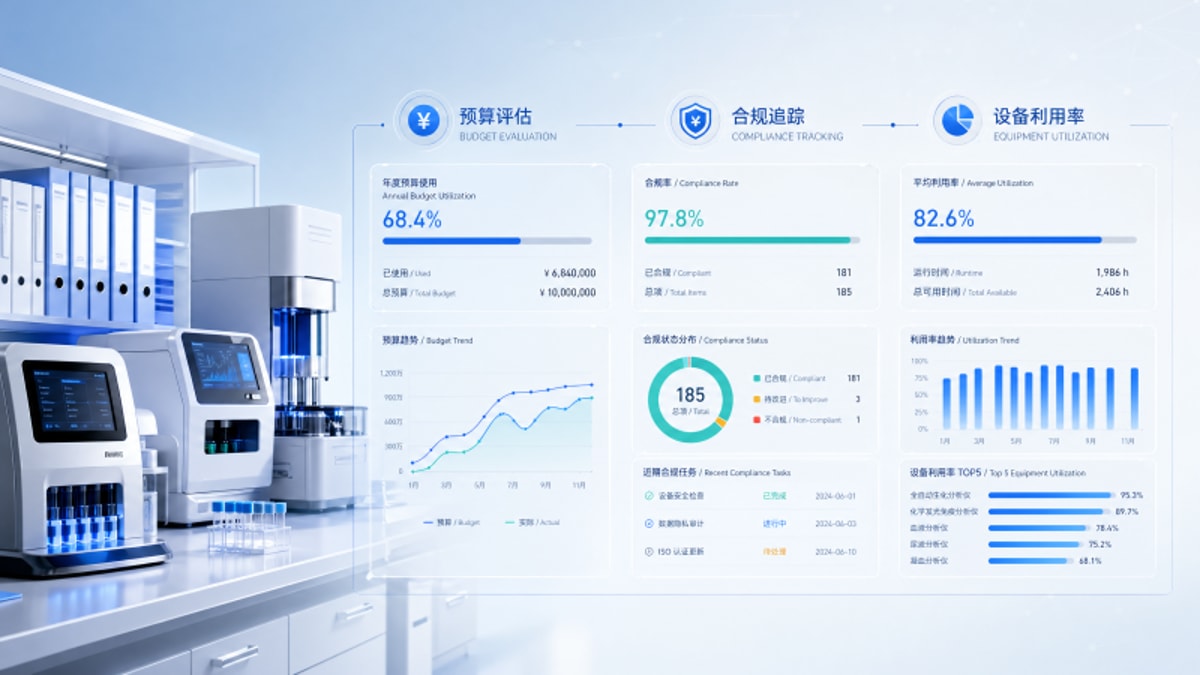
In an environment where every healthcare dollar must prove its value, healthcare analytics helps financial decision-makers move beyond assumptions and toward evidence-based budget planning. By connecting cost, utilization, compliance, and performance data, organizations can identify which investments reduce risk, improve operational efficiency, and support long-term outcomes—making every budget call smarter, more defensible, and aligned with strategic healthcare priorities.
Why a checklist approach makes healthcare analytics more useful for budget approval
For finance approvers, the main challenge is rarely a lack of dashboards. The problem is deciding which signals deserve attention before capital is allocated, vendor contracts are renewed, or a digital health project moves from pilot to scale. A checklist-based approach to healthcare analytics reduces noise and creates a repeatable review method that can be applied across devices, lab systems, care pathways, and infrastructure planning.
This matters even more in healthcare procurement cycles that often stretch from 3 to 12 months, especially when technical evaluation, regulatory review, and interoperability checks happen in parallel. Budget decisions made too early can lock institutions into underperforming technology. Decisions made too late can delay operational improvement, compliance readiness, or service expansion. A disciplined healthcare analytics framework helps balance both timing and evidence.
For organizations operating in a value-based environment, the best budget calls usually connect five dimensions: cost, utilization, technical performance, risk exposure, and long-term maintainability. That is why procurement directors, CFO teams, laboratory planners, and operational leaders increasingly use structured review criteria instead of relying on vendor claims alone.
What finance teams should confirm before reviewing any analytics report
- Whether the data covers a meaningful observation period, such as 6, 12, or 24 months, rather than a short-term snapshot.
- Whether the metrics include both direct costs and downstream effects, including rework, service calls, training time, and compliance-related delays.
- Whether utilization data is normalized by department, patient volume, device class, or test throughput so comparisons are fair.
- Whether technical performance indicators can be traced to engineering or operational evidence rather than presentation-level summaries.
When these basics are missing, healthcare analytics may still look polished, but it becomes weak support for budget approval. Financial decision-makers need defensible numbers that stand up under audit, committee review, and post-purchase evaluation.
The core healthcare analytics checklist for smarter budget calls
A practical budget review should begin with a short list of metrics that translate technical reality into financial relevance. In healthcare analytics, the most useful metrics are rarely the most fashionable ones. Finance approvers usually benefit more from stability, traceability, and risk-linked measures than from abstract AI scoring or isolated growth charts.
The table below highlights a budget-focused review structure that can be used when comparing medical technologies, diagnostic systems, digital platforms, or service contracts. It is especially relevant when multiple departments are competing for the same annual budget window.
Used together, these categories turn healthcare analytics into a decision tool rather than a reporting exercise. For example, a lower-cost system may appear attractive until service frequency, consumable dependency, or integration effort is modeled across a 36-month operating horizon. In many cases, the financially safer choice is not the lowest bid, but the option with stronger reliability and clearer compliance documentation.
Priority checks for a finance-first review
- Confirm whether the baseline cost problem is real, recurring, and measurable.
- Check whether utilization trends justify buying new capacity versus optimizing existing assets.
- Evaluate whether technical performance supports stable operation under normal and peak workloads.
- Map compliance requirements before assigning budget, especially for regulated device categories.
- Ask for evidence that the projected savings can be tracked after implementation at 90, 180, and 365 days.
A practical threshold question
If a proposal cannot show which metric will improve, by how much, and over what time frame, it is not yet ready for budget approval. That simple rule screens out a large share of weak business cases before they consume internal review time.
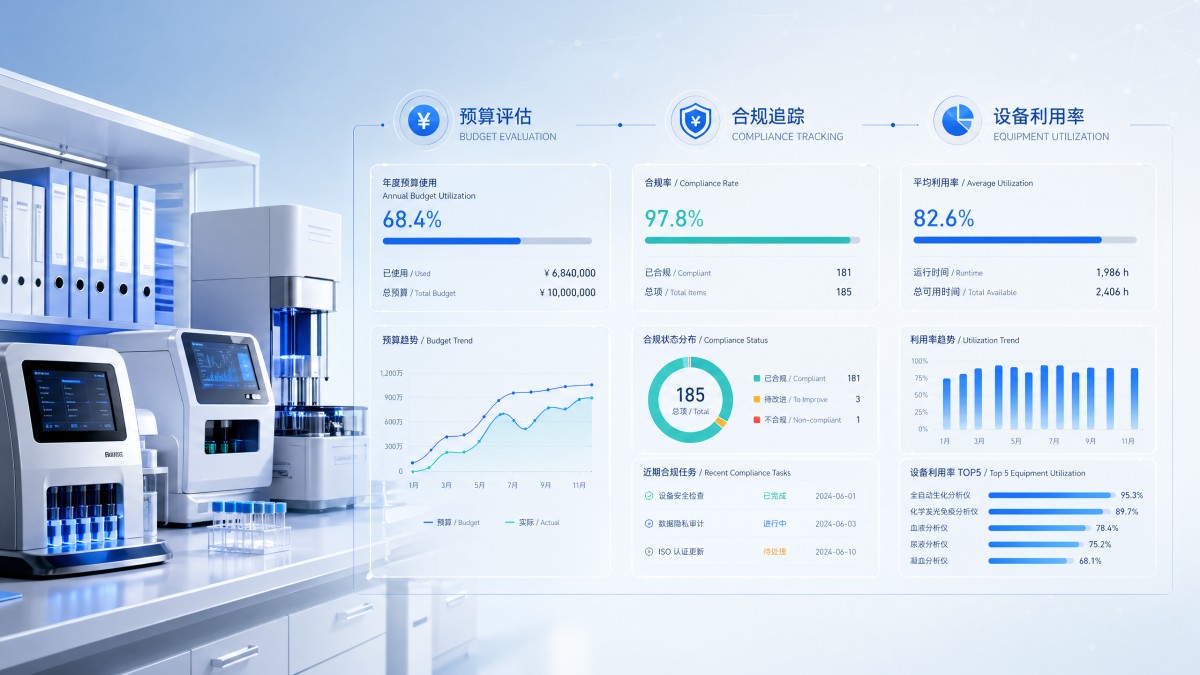
How to judge metrics differently across procurement, laboratories, and digital health projects
Not every healthcare analytics metric carries the same weight in every scenario. A hospital procurement team evaluating implant-related equipment will prioritize reliability and material performance risk differently than a laboratory architect evaluating throughput variability or instrument integration. Financial approval becomes stronger when the metric set is adapted to the operational context.
This is where independent technical benchmarking becomes valuable. VitalSync Metrics supports decision-makers by translating engineering parameters into standardized review material, making it easier to compare options that are often marketed with inconsistent terminology. For budget owners, this reduces the chance of approving spend based on incomplete or non-equivalent claims.
The comparison below shows how healthcare analytics priorities often shift by application area. The goal is not to create separate silos, but to make sure the budget case reflects the real operating pressure point.
For finance approvers, the lesson is straightforward: healthcare analytics should not be evaluated as a generic reporting function. It should be matched to the type of budget decision under review. In many organizations, that single adjustment improves approval quality more than adding more dashboards or more software licenses.
Scenario-based review prompts
- For procurement: Are we funding performance, or just acquiring inventory?
- For laboratories: Does the metric set capture throughput under real working conditions, not only ideal test conditions?
- For digital monitoring: Can the data quality support action without creating extra false alerts or clinical review burden?
- For long-life devices: Is the engineering evidence strong enough to reduce future replacement or nonconformance cost?
Common blind spots that weaken budget decisions
Even mature organizations can misuse healthcare analytics when budget pressure is high. The most common problem is overvaluing acquisition price while undervaluing risk transfer. A lower upfront price can become more expensive within 12 to 24 months if downtime, consumables, retraining, or technical drift are not modeled early.
Another blind spot is treating compliance as a separate legal or quality issue rather than a budget variable. In reality, documentation gaps, delayed technical files, unclear labeling, and weak traceability can affect launch timing, contract readiness, and internal validation costs. For regulated healthcare environments, compliance readiness should be included in the financial model from the beginning.
A third issue is accepting performance claims without engineering context. Metrics such as accuracy, sensitivity, durability, or stability can be presented in favorable terms, yet still fail to reflect daily operating conditions. Independent benchmarking helps reduce this risk by converting technical claims into comparable evidence.
Blind spots worth flagging in every approval meeting
- A business case that uses only purchase price and ignores 3-year service and support cost.
- Analytics reports built on short pilot windows of fewer than 90 days when the full usage pattern is seasonal or department-dependent.
- Utilization figures that do not distinguish between peak occupancy and normal baseline volume.
- Vendor comparisons that use inconsistent definitions for uptime, throughput, or maintenance burden.
- No post-approval review plan to confirm whether expected savings actually materialize within the first 6 or 12 months.
A useful control question
If the project under review underperforms by 10% to 15%, which budget line absorbs the impact? Asking this question forces teams to reveal whether the risk is already priced into the proposal or silently pushed into operations.
A step-by-step review method finance approvers can apply immediately
A strong healthcare analytics process does not need to be complicated. What it does need is discipline. Finance teams can use a five-step review method to screen proposals before deeper committee review. This improves speed, consistency, and accountability across capital requests and strategic sourcing decisions.
The most effective reviews usually combine quantitative metrics with a structured technical note. That technical note should explain how performance data was generated, what assumptions were used, and where uncertainty remains. For high-impact procurement, this can save weeks of back-and-forth later in the approval cycle.
Below is a practical review sequence that works well for hospitals, diagnostic networks, MedTech evaluation teams, and laboratory planning groups.
Five-step decision checklist
- Define the budget question clearly: replacement, expansion, risk reduction, capacity increase, or compliance upgrade.
- Select 4 to 6 metrics that directly relate to that question, such as utilization, failure rate, throughput, service burden, or documentation readiness.
- Review the time horizon: short-term effect at 90 days, operational effect at 6–12 months, and lifecycle effect at 3–5 years.
- Stress-test assumptions using downside cases, including lower adoption, higher maintenance frequency, or delayed integration.
- Document approval conditions, including performance checkpoints and evidence required after deployment.
This process keeps healthcare analytics tied to real budget outcomes. It also helps create a common language between finance, operations, procurement, engineering, and quality teams. That cross-functional alignment is often the difference between a fast approval and a stalled one.
What to prepare before requesting external benchmarking support
If your team plans to use external benchmarking or technical validation, prepare the current system baseline, expected operating range, known compliance constraints, and the top 3 budget concerns. In many cases, that includes service frequency, integration friction, performance drift, or uncertainty around MDR/IVDR-related documentation expectations.
Having those inputs ready allows the analytics review to move from descriptive reporting to decision-grade insight. It also ensures that the final recommendation is anchored in the organization’s actual risk profile rather than in generic market language.
Why decision-makers work with VitalSync Metrics
VitalSync Metrics supports healthcare leaders who need more than promotional claims when budget decisions involve technical complexity. Our role is to act as an independent, data-driven filter for the MedTech and Life Sciences supply chain, translating engineering performance into standardized evidence that finance approvers can actually use.
Whether you are reviewing wearable sensor signal quality, laboratory system consistency, implant material endurance, or broader healthcare analytics inputs for procurement, VSM helps convert raw technical parameters into clearer budget intelligence. That means better support for sourcing confidence, stronger internal approval discussions, and more realistic lifecycle planning.
If you need to evaluate options before releasing budget, contact us to discuss the exact points that matter to your approval process. We can help you clarify technical parameters, compare solution paths, review delivery timelines, assess documentation readiness, and structure a more defensible investment case.
What you can contact us about
- Parameter confirmation for device, laboratory, or digital health performance claims
- Product or system selection support based on budget-sensitive evaluation criteria
- Estimated delivery cycle planning for validation, procurement, or phased deployment
- Custom benchmarking scope built around your risk, compliance, or utilization concerns
- Certification and documentation review priorities relevant to MDR, IVDR, or technical traceability
- Early-stage quotation discussions tied to measurable decision criteria rather than broad assumptions
Next step
If your organization is trying to make healthcare analytics more useful for budget approval, start with the metrics that expose cost, risk, and operational reality at the same time. When those inputs are independently validated and clearly structured, budget calls become faster, smarter, and easier to defend. Contact VitalSync Metrics to discuss your evaluation scope, technical questions, budget priorities, and the evidence you need before moving forward.
Recommended News
- 2026.04.29Healthcare Analytics Metrics That Support Smarter Budget CallsLydia Vancini (Regulatory Compliance Lead)
- 2026.04.29Mobility Assist Selection Mistakes That Limit Long-Term UseSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.04.29Endoscope Image Resolution Benchmark for Vendor ComparisonDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
