Smart orthotics vs traditional braces: key differences

As wearable healthcare technology reshapes orthopedic care, understanding the gap between smart orthotics and traditional braces is essential for users, buyers, and healthcare decision-makers. This guide explores how medical technology advancements, healthcare compliance solutions, and medical equipment safety standards influence comfort, monitoring, durability, and long-term value—helping readers evaluate which option better fits modern clinical and mobility needs.
For procurement teams, clinicians, rehabilitation operators, and MedTech evaluators, the comparison is no longer limited to basic support versus no support. The real question is whether a device can deliver measurable outcomes, maintain safety under daily load, integrate with digital monitoring workflows, and remain reliable over a 6–24 month usage cycle.
This matters in a market where value-based purchasing is becoming standard. Buyers increasingly need evidence on fit stability, sensor accuracy, battery endurance, material fatigue, cleaning requirements, and data governance. In that context, smart orthotics and traditional braces serve overlapping but distinctly different roles.
Understanding the Core Difference Between Smart Orthotics and Traditional Braces
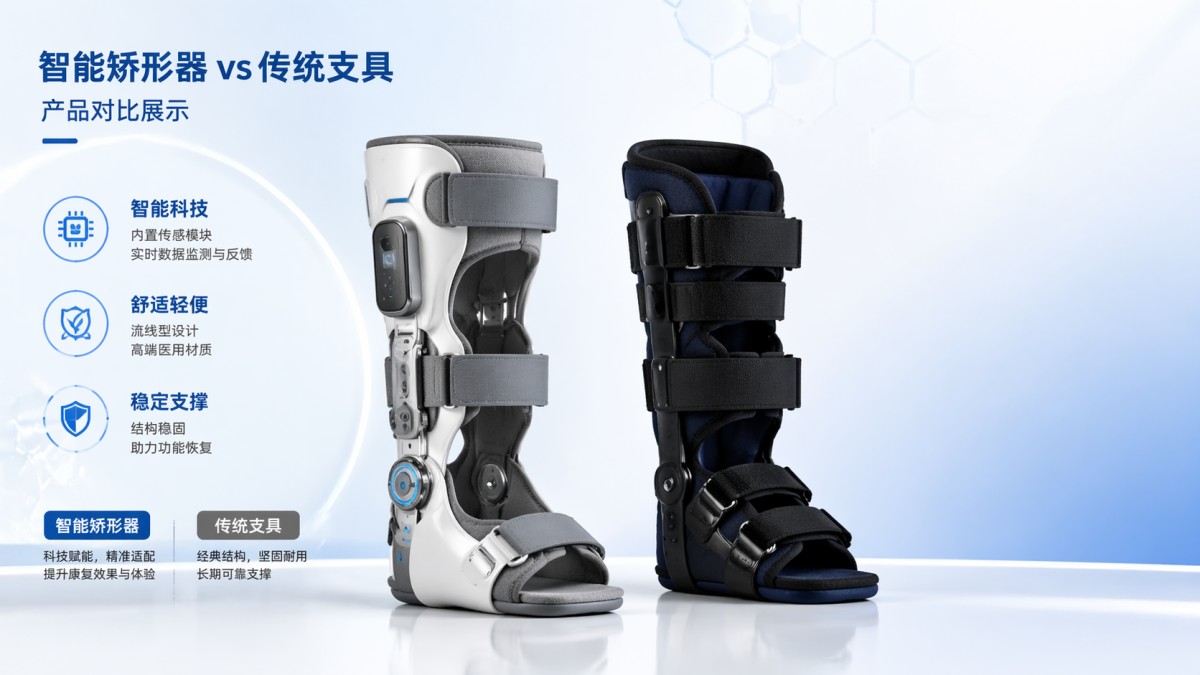
Traditional braces are primarily passive support devices. They stabilize a joint, reduce motion, redistribute load, or protect injured tissue during recovery. Common formats include knee braces, ankle braces, wrist supports, and spinal braces made from textiles, polymers, metal stays, or composite shells. Their value is mechanical: support, protection, and basic alignment control.
Smart orthotics add a digital layer to that mechanical function. In addition to structural support, they may include pressure sensors, inertial measurement units, motion tracking modules, microcontrollers, and in some cases wireless connectivity. Instead of offering only support, they can capture gait data, usage adherence, pressure distribution, and range-of-motion trends over time.
This difference becomes important when outcomes must be monitored. A passive brace can help immobilize or guide movement, but it usually cannot confirm whether the user wore it for 8 hours per day, whether alignment drift increased after 3 weeks, or whether load asymmetry suggests a worsening compensatory gait pattern.
In rehabilitation and chronic musculoskeletal management, these details affect both clinical and commercial decisions. For a hospital or distributor, smart orthotics may justify a higher upfront cost if they reduce follow-up visits, improve adherence, or provide evidence for therapy adjustments. For lower-risk cases, a traditional brace may remain the more efficient option.
How the two categories are typically positioned
The practical distinction can be summarized by function scope. Traditional braces focus on 1 core task: mechanical stabilization. Smart orthotics usually cover 3 layers at once: support, data capture, and feedback. That broader scope can benefit orthopedic care, but it also introduces new requirements in software validation, charging, cleaning, and data management.
The table below outlines the main functional differences relevant to operators and procurement teams evaluating orthopedic support devices.
- ESS
- healthcare technology
- connected car
- EdTech
- procurement
- AR
- Cement
- material fatigue
- medical technology
- medical equipment
- material fatigue
- healthcare technology
- healthcare compliance
- Smart Orthotics
- medical technology advancements
- medical equipment safety standards
- wearable healthcare technology
- healthcare compliance solutions
Recommended News
- 2026.04.24Medical technology cost: where budgets go wrongDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.04.24Packaging choices that protect sterile instrumentsDr. Julian Rossi (RehabTech Specialist)
- 2026.04.24Mobility assist devices: which option fits bestSarah Jenkins (Laboratory Infrastructure Consultant)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
