Wearable healthcare technology: who benefits most
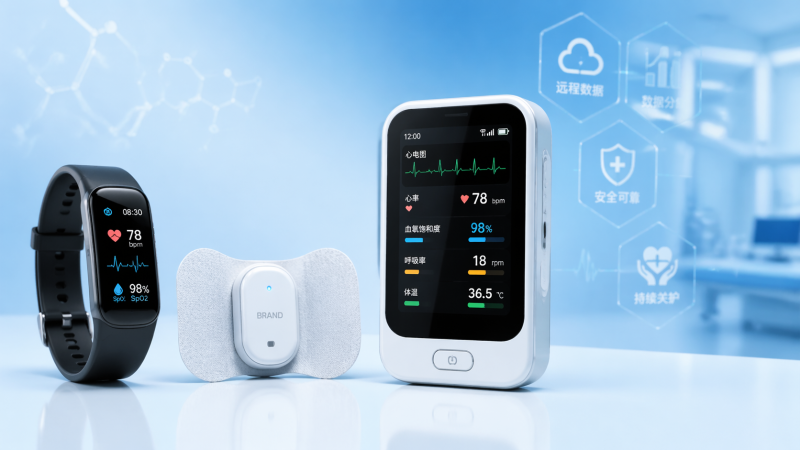
Wearable healthcare technology benefits many stakeholders, but not equally. The biggest gains usually go to groups that can turn continuous data into action: clinicians managing high-risk patients, operators responsible for workflow and safety, procurement teams validating product performance, and decision-makers balancing outcomes against cost and compliance. For these readers, the key question is not whether wearables are innovative—it is where they create measurable value, what risks they introduce, and how to judge whether a device is truly fit for clinical or operational use.
As medical technology advancements continue, wearable systems are moving beyond consumer wellness into hospital monitoring, rehabilitation, remote care, staff safety, and laboratory environments. That shift raises practical questions around healthcare compliance solutions, medical equipment safety standards, interoperability, durability, and medical technology cost. The organizations that benefit most are those that evaluate wearable technology with engineering discipline rather than marketing assumptions.
Who benefits most from wearable healthcare technology in practice?
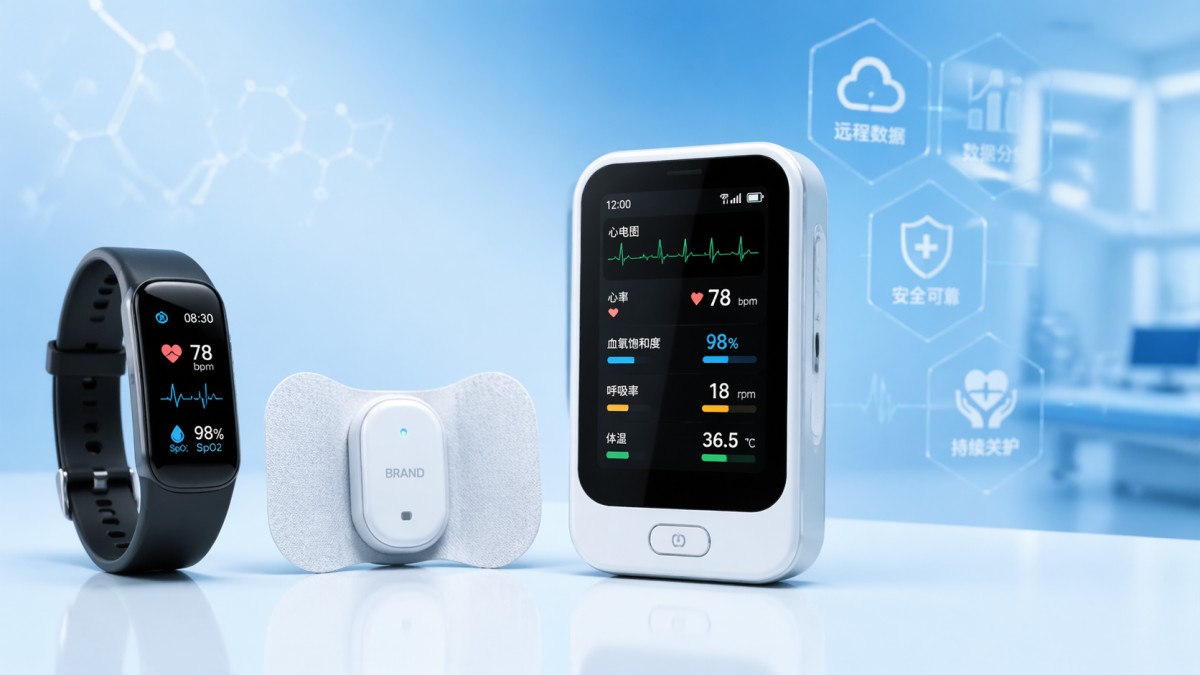
The short answer: the highest value goes to users and organizations dealing with continuous monitoring, time-sensitive intervention, and performance accountability.
1. Clinicians and care teams
Clinicians benefit most when wearable healthcare technology helps detect deterioration earlier, reduce blind spots between spot checks, and support better decisions with trend data rather than isolated readings. This is especially useful in:
- Post-acute recovery monitoring
- Cardiac and respiratory observation
- Chronic disease management
- Rehabilitation progress tracking
- Elderly and high-risk patient supervision
If a wearable device can reliably capture motion, heart rate, oxygen saturation, temperature, sleep quality, or adherence patterns, care teams can intervene sooner and prioritize attention more effectively. The benefit is strongest where staffing is stretched and patient risk changes quickly.
2. Hospital operators and frontline users
Operators benefit when wearable systems reduce manual checks, simplify documentation, improve patient throughput, or add visibility into workflow and safety. For example, continuous monitoring can reduce gaps in observation during transport, recovery, or lower-acuity settings. In some environments, staff wearables can also support fatigue management, location awareness, ergonomic risk reduction, or infection-control workflows.
For this group, usability matters as much as accuracy. A wearable that is difficult to charge, sanitize, fit, calibrate, or integrate into daily routines may fail operationally even if its technical specifications look strong.
3. Procurement leaders and sourcing teams
Procurement benefits when wearable healthcare technology can be evaluated objectively. This group often faces the largest gap between product claims and real-world performance. Their advantage comes from selecting devices that meet technical thresholds, regulatory expectations, and lifecycle requirements before deployment problems appear.
For buyers, the real value is risk reduction. A better purchasing decision can lower:
- Replacement and maintenance costs
- Integration failures
- False alarms or poor signal quality
- Compliance exposure
- User adoption problems
- Long-term total cost of ownership
4. Business decision-makers and innovators
Executives, innovation teams, and MedTech developers benefit when wearables create strategic advantages: better patient outcomes, stronger service models, differentiated offerings, and more efficient care delivery. But these gains only hold if the underlying technology is clinically credible and scalable.
In other words, wearable healthcare technology delivers the greatest benefit where data reliability, workflow fit, and measurable outcomes align.
What do target readers care about most before they trust the value?
Across information researchers, users, procurement professionals, and enterprise leaders, the same concerns appear repeatedly.
Is the data accurate enough for healthcare use?
This is the first filter. Many wearable products can generate data, but not all can generate decision-grade data. Readers want to know whether the device performs consistently across motion, skin types, clinical conditions, ambient interference, and prolonged use.
Does it support compliance and safety requirements?
Healthcare buyers are increasingly concerned with healthcare compliance solutions, including MDR/IVDR alignment where applicable, cybersecurity, traceability, biocompatibility, and documentation quality. Medical equipment safety standards are not a side issue—they are a purchasing and deployment barrier if not addressed early.
Will it fit into real workflows?
Frontline users do not want another device that creates alert fatigue, extra charging cycles, poor patient comfort, or disconnected data streams. Procurement and management teams also want proof that implementation will not overload IT, nursing, biomedical engineering, or laboratory staff.
What is the actual cost beyond the purchase price?
Medical technology cost is a major concern, especially in value-based procurement environments. Readers want to understand software fees, sensor replacement cycles, calibration needs, accessories, training, integration effort, downtime risk, and support response times.
Which patient groups or use cases benefit enough to justify investment?
Wearables are not universally high-value. Their impact depends on acuity level, care model, staffing constraints, and intervention pathways. Decision-makers want to know where the return is real, and where it may be overstated.
Where does wearable healthcare technology create the clearest value?
Not every use case delivers the same return. The strongest applications usually share one trait: continuous, actionable insight leads to better decisions or lower operational burden.
Remote patient monitoring
This remains one of the clearest value areas. Wearables help extend visibility beyond hospital walls, enabling earlier detection of deterioration and better management of chronic conditions. The benefit is particularly strong when there is an established escalation pathway and staff can act on alerts.
Step-down and lower-acuity observation
In settings where full bedside monitoring is not always practical, wearables can help maintain oversight without the infrastructure intensity of traditional systems. This can support resource efficiency while preserving patient safety.
Post-surgical recovery and rehabilitation
Wearables can track mobility, recovery milestones, adherence, and physiological trends. For providers, this improves continuity; for patients, it can increase engagement and provide reassurance.
Elder care and high-risk populations
Fall detection, movement analysis, sleep monitoring, and adherence support can create meaningful benefits in elderly care and long-term supervision. However, success depends heavily on comfort, battery life, false alarm control, and ease of use.
Staff safety and operational performance
In some healthcare and laboratory environments, wearables also support workforce safety by monitoring fatigue, environmental exposure, posture, movement strain, or access patterns. This value is often under-discussed but can be important for occupational health and process optimization.
How should buyers judge whether a wearable is genuinely worth adopting?
For procurement teams and decision-makers, the best evaluation approach is not feature comparison alone. It is multi-layered technical and operational validation.
Assess signal quality, not just claimed accuracy
A wearable may advertise high performance under ideal conditions, but real healthcare settings introduce motion, poor placement, perspiration, variable anatomy, and electromagnetic noise. Buyers should ask for evidence on signal-to-noise ratio, artifact handling, drift behavior, and consistency over time.
Validate clinical relevance
A technically impressive metric is not automatically clinically useful. The important question is whether the data supports intervention, prioritization, diagnosis support, or workflow improvement in a meaningful way.
Review regulatory and documentation maturity
Strong products should come with clear technical files, intended use definitions, safety evidence, material information, and compliance documentation. Weak documentation is often a warning sign, especially when scaling across regulated markets.
Examine integration demands
Even strong devices can fail commercially if they do not fit with EMR systems, hospital IT architecture, alarm strategies, maintenance routines, and cybersecurity policies. Integration complexity should be treated as part of the product cost.
Calculate lifecycle economics
Medical technology cost should include:
- Initial hardware and software
- Consumables and replacement parts
- Maintenance and recalibration
- Training time
- IT integration effort
- Downtime and support risks
- Upgrade and obsolescence exposure
Run pilot programs with measurable endpoints
Before broad rollout, organizations should test wearables in a defined setting with success metrics such as reduced observation gaps, lower readmission risk, improved patient adherence, fewer adverse events, or lower manual workload. Without measurable endpoints, “innovation” is hard to defend.
Who benefits less, or only under specific conditions?
Some stakeholders benefit only when the surrounding system is ready.
Patients without support pathways
If data is collected but no care pathway exists to interpret and act on it, the patient benefit is limited. Wearables are not valuable simply because they monitor; they are valuable when monitoring changes care.
Organizations with weak data governance
Without clear policies for data quality, privacy, interoperability, and alert management, wearables may create complexity instead of improvement.
Teams adopting devices for trend appeal rather than operational fit
Some technologies are purchased because they appear future-facing, not because they solve a pressing workflow or outcome problem. In these cases, adoption rates and ROI often disappoint.
Environments where durability is underestimated
Healthcare and laboratory use puts stress on materials, charging systems, fastening methods, adhesives, and sensors. Devices that perform well in demos may degrade quickly in demanding environments if fatigue limits and environmental tolerances are not properly validated.
Why data-driven benchmarking matters more as the market matures
As wearable healthcare technology grows more sophisticated, buyers face a wider spread in quality. Some products are built for consumer engagement; others are engineered for regulated, clinical-grade use. The difference is not always obvious from brochures or surface-level specifications.
This is why independent benchmarking matters. Data-driven evaluation helps organizations compare products on engineering truth rather than promotional positioning. That includes not only performance metrics, but also material resilience, reliability under stress, regulatory maturity, and long-term operational viability.
For procurement directors, this supports stronger sourcing decisions. For operators, it reduces implementation friction. For innovators, it clarifies where product development must improve. For decision-makers, it creates a more defensible path between investment and outcome.
Conclusion: the biggest winners are those who can turn wearable data into better decisions
Wearable healthcare technology benefits many groups, but the greatest value goes to clinicians, operators, procurement teams, and healthcare leaders who can connect device data to action, safety, and measurable performance. The strongest benefits appear in remote monitoring, recovery, chronic care, workforce safety, and settings where continuous visibility improves intervention or efficiency.
However, value does not come from novelty alone. It comes from verified performance, workflow compatibility, healthcare compliance solutions, adherence to medical equipment safety standards, and a realistic understanding of medical technology cost over the full lifecycle.
For organizations evaluating wearables today, the best question is not “Who can use this?” but “Who can benefit measurably, safely, and sustainably?” The answer depends on whether the technology has been tested with enough rigor to earn trust in real healthcare environments.
- Wearable technology
- EMS
- ESS
- PPE
- healthcare technology
- patient monitoring
- remote monitoring
- EdTech
- procurement
- cybersecurity
- AR
- Cement
- benchmarking
- value-based procurement
- medical technology
- medical equipment
- signal-to-noise ratio
- engineering truth
- data-driven
- biomedical engineering
- healthcare technology
- healthcare compliance
- Remote Monitoring
- medical technology cost
- medical technology advancements
- medical equipment safety standards
- wearable healthcare technology
- healthcare compliance solutions
Recommended News
- 2026.04.24Medical technology cost: where budgets go wrongDr. Alistair Thorne (Senior Biomedical Engineer)
- 2026.04.24Packaging choices that protect sterile instrumentsDr. Julian Rossi (RehabTech Specialist)
- 2026.04.24Mobility assist devices: which option fits bestSarah Jenkins (Laboratory Infrastructure Consultant)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
