Surgical Instrument Kits OEM: How to Judge Supplier Fit
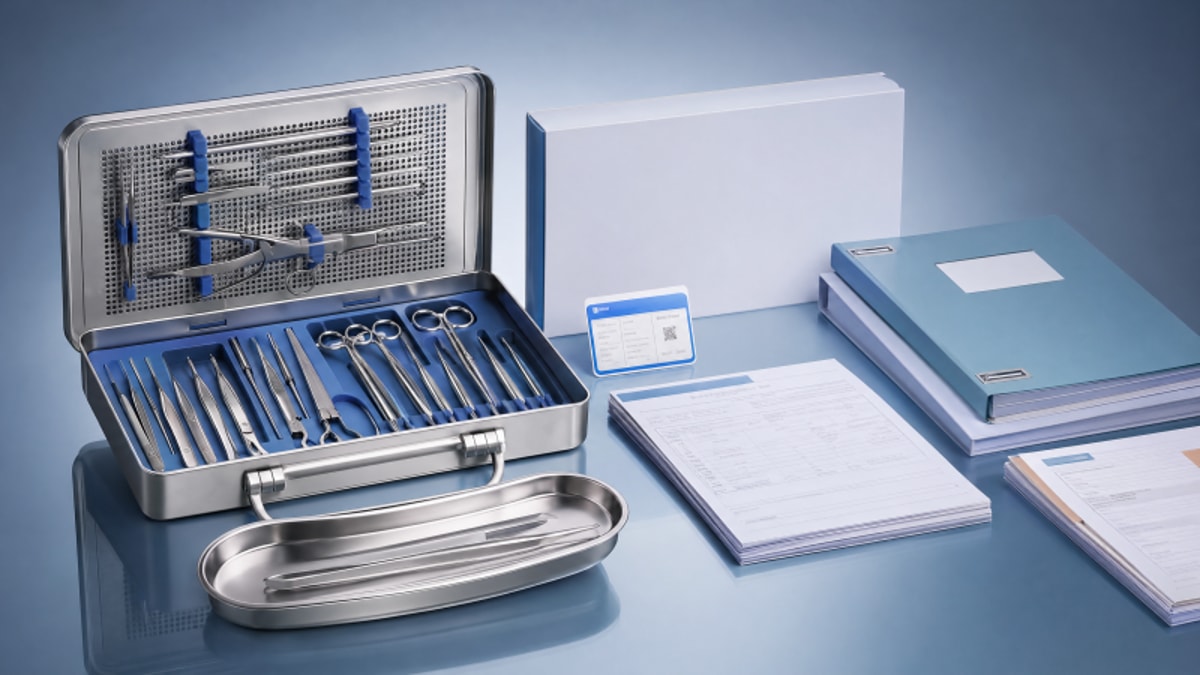
Choosing a surgical instrument kits OEM is not just about price or production capacity—it is about proving technical consistency, regulatory readiness, and long-term supply reliability. For procurement professionals, the real question is how to identify a supplier that aligns with clinical expectations and business risk controls. This guide explains the key criteria to judge supplier fit with greater confidence.
Why supplier fit changes by procurement scenario
In the market for surgical instrument kits OEM services, the same supplier may be a strong fit for one buyer and a poor fit for another. A regional distributor seeking stable repeat orders of 500 to 2,000 kits per quarter will judge fit differently from a MedTech startup validating a new procedural set, or a hospital group that needs standardized kits across 3 to 20 facilities. Procurement teams should therefore start with the scenario, not the catalog.
This matters because surgical instrument kits combine multiple technical and operational variables: material grade, surface finish, passivation, dimensional tolerances, tray configuration, sterilization compatibility, labeling, packaging validation, and traceability. A supplier that offers attractive unit pricing may still fail on lot consistency, documentation depth, or change control discipline. In healthcare procurement, those gaps often create larger downstream costs than a 5% to 12% purchase price difference.
For buyers working in regulated healthcare supply chains, supplier fit should be judged through risk exposure over a 12- to 36-month horizon. That includes lead-time stability, nonconformance handling, design transfer capability, and the ability to support technical files when market requirements evolve. In practical terms, the best surgical instrument kits OEM partner is the one that matches your usage environment, documentation burden, and supply continuity needs.
Three common buyer situations
- Hospital or IDN procurement: priority is standardization, replenishment reliability, and low field disruption.
- Distributor or private label buyer: priority is cost control, packaging flexibility, and scalable supply across multiple SKUs.
- MedTech startup or procedural innovator: priority is engineering collaboration, iterative prototyping, and design documentation.
When these situations are not separated early, procurement teams often compare suppliers on incomplete criteria. A useful sourcing process begins by assigning weight to at least 4 dimensions: technical quality, compliance readiness, supply resilience, and commercialization support. Only then can a surgical instrument kits OEM evaluation become consistent and defensible.
Scenario 1: Hospital networks and centralized procurement programs
In a hospital group or centralized procurement environment, surgical instrument kits OEM selection is usually driven by repeatability more than novelty. The concern is not whether a supplier can build one acceptable sample set, but whether it can maintain kit accuracy, finish quality, and replenishment timing over 12 monthly cycles or multi-year contracts. For this scenario, procurement should test process discipline before discussing scale discounts.
Hospital buyers also need to account for how kits are used across departments. A general surgery tray, a minor procedure set, and a specialty instrument kit may all require different cleaning workflows, replacement frequency, and handling protocols. If a supplier cannot document component-level traceability, part substitution rules, and packaging consistency, the operational burden shifts to sterile processing teams and materials management staff.
A practical benchmark in this setting is to ask whether the supplier can maintain agreed kit configuration accuracy across at least 3 consecutive production lots, while also supporting routine replenishment lead times in the 6- to 10-week range. Even where exact timing varies by geography, a supplier should be able to explain which steps drive lead time and where bottlenecks typically appear.
What matters most in this scenario
Operational fit indicators
- Stable bill of materials and clear controls for component replacement or approved equivalents.
- Consistent packaging and labeling formats that support internal receiving and storage processes.
- Defined complaint handling and corrective action workflow, ideally with response milestones inside 48 to 72 hours for urgent issues.
- Evidence that sterilization compatibility, corrosion resistance, and cleaning durability have been considered at kit level, not just per instrument.
For hospital buyers, the strongest surgical instrument kits OEM partner is usually not the one with the broadest brochure. It is the one that can map manufacturing controls to clinical continuity. If a supplier cannot explain how it manages incoming material verification, in-process inspection, and final kit reconciliation, procurement should treat that as a warning signal.
The comparison below helps buyers align evaluation criteria with real use environments rather than generic sourcing claims.
This table shows why supplier fit should not be judged by a single score. A surgical instrument kits OEM that works well for centralized hospital procurement must prove repeatable process control, while another buyer may prioritize labeling options or design iteration speed. The procurement framework needs to reflect that difference explicitly.
Scenario 2: Distributors, importers, and private label programs
For distributors and private label buyers, surgical instrument kits OEM sourcing is often a portfolio decision rather than a one-off purchase. The supplier must support multiple kit structures, packaging variations, and commercial rollouts across different channels. In this scenario, procurement teams should examine whether the supplier can maintain quality while handling SKU complexity, forecast swings, and brand-specific documentation.
A common mistake is to focus only on ex-works price. For distribution businesses, hidden cost often sits in packaging revisions, relabeling delays, low forecast visibility, accessory shortages, or quality escapes that trigger returns. A supplier that is 8% cheaper at purchase order stage may become more expensive when total landed cost and service burden are measured over 2 to 4 quarters.
This is also the scenario where MOQ, shelf presentation, language requirements, and market-specific compliance labeling matter most. Buyers should ask how many packaging versions a supplier can manage without raising error rates, what the standard approval cycle is for artwork changes, and whether component substitutions require pre-approval. Strong suppliers answer these questions in process terms, not sales language.
Questions distributors should ask early
- What is the realistic MOQ by kit type, not just by instrument family?
- How are artwork approvals, label revisions, and carton changes controlled?
- Can the supplier separate prototype, pilot, and commercial production documentation?
- What are the standard lead times for first order, repeat order, and urgent replenishment?
- How are shortages, back orders, and alternative sourcing decisions communicated?
In practice, the best surgical instrument kits OEM partner for a distributor is often one with disciplined planning communication. A supplier that can support rolling 90-day forecasts, lock critical components earlier in the cycle, and issue timely change notices usually reduces channel disruption more effectively than one that simply promises fast production.
Scenario 3: MedTech startups and procedure-specific kit development
A startup developing a procedure pack or specialized surgical set needs a different kind of surgical instrument kits OEM relationship. Here, the critical issue is not just manufacturing output but engineering translation. The supplier must understand how clinical intent becomes manufacturable specifications, including material choices, ergonomic features, tray geometry, and packaging constraints that support usability and transport.
In early-stage projects, buyers should expect at least 2 to 4 revision cycles before a kit reaches stable pilot form. That makes revision control, design history support, and sample evaluation turnaround more important than headline capacity. If a supplier struggles to document version changes, tolerance updates, or component rationale, procurement risk increases as the program moves toward verification and market preparation.
This scenario also requires sharper scrutiny of regulatory readiness. While the OEM may not be the legal manufacturer in every business model, its documentation quality can still influence technical file preparation, risk assessments, and supplier qualification outcomes. A startup should therefore ask what level of material certificates, process records, and inspection evidence can be provided routinely rather than exceptionally.
What “engineering fit” looks like
High-value indicators during sampling and pilot build
- The supplier can translate clinical use inputs into manufacturable drawings or controlled specifications.
- Prototype feedback is documented with measurable recommendations, not only subjective comments.
- Pilot lots are separated from commercial lots with clear revision status and acceptance criteria.
- The OEM can define which features are critical to function, which are cosmetic, and which need validation support.
A capable surgical instrument kits OEM in this environment behaves more like a process partner than a simple fabricator. Procurement should look for evidence of structured technical communication, especially during the first 8 to 16 weeks of project ramp-up. That period often reveals whether the supplier can support long-term commercialization or only early sampling.
How to compare suppliers across quality, compliance, and supply risk
Once the business scenario is clear, procurement needs a comparison framework that converts supplier claims into verifiable checkpoints. In healthcare-related sourcing, it is useful to score each surgical instrument kits OEM across at least 5 areas: manufacturing controls, documentation quality, regulatory support, supply continuity, and commercial responsiveness. Even a simple weighted matrix can improve decision quality if it is applied consistently.
Quality should include more than final inspection. Buyers should ask about incoming material verification, passivation or finishing control where applicable, in-process checks, final kit reconciliation, and handling of rework. Compliance support should cover whether the supplier can provide material records, lot traceability, labeling control documentation, and change notification discipline. Supply continuity should examine dual sourcing logic for critical parts, production planning visibility, and realistic lead-time performance.
Below is a practical scoring structure procurement teams can adapt. The exact weighting will vary, but the discipline of comparing suppliers on defined evidence usually exposes weak fit faster than price negotiation alone.
This type of matrix supports balanced decisions. A surgical instrument kits OEM should not be selected on commercial terms alone if documentation or process control is weak. In healthcare procurement, the cost of one unresolved quality event can outweigh the savings from a lower initial quote.
Common misjudgments during supplier selection
One frequent misjudgment is assuming that sample acceptance proves scale readiness. A supplier may produce a high-quality pilot kit with extra manual oversight, yet struggle when monthly volume rises from 50 sets to 500 sets. Procurement should always ask how pilot controls transition into routine production controls, and whether quality performance is monitored by lot, by component, or only at shipment stage.
Another mistake is treating compliance as paperwork only. For surgical instrument kits OEM projects, documentation quality is often a proxy for process maturity. Weak change control, inconsistent part naming, or unclear material records usually point to broader execution risk. If documentation takes repeated follow-up, that issue should be weighted in the sourcing decision rather than tolerated as an administrative inconvenience.
A third misjudgment is underestimating supply resilience. Buyers may overlook single-source dependencies for inserts, trays, fasteners, or packaging components. Yet these details often determine whether a supplier can maintain a 95%+ service level during demand fluctuation or logistics disruption. Asking about critical component planning is a practical way to test real operational maturity.
A practical qualification checklist for procurement teams
To judge surgical instrument kits OEM fit with fewer blind spots, procurement teams should use a staged qualification approach. This does not need to be overly complex. In many cases, a 3-step process covering technical review, sample or pilot evaluation, and commercial-risk review can create enough evidence for a sound decision. The key is to define acceptance criteria before supplier discussions become price-led.
The first stage should verify baseline fit: product scope, material expectations, documentation availability, and target lead times. The second stage should assess whether the supplier can reproduce kit integrity across samples or pilot lots. The third stage should review forecast handling, communication routines, escalation paths, and contract-level details such as change notice expectations or packaging approval controls.
When this structure is used, buyers can compare two or three suppliers more objectively. It also helps internal stakeholders align faster, especially when quality, regulatory, operations, and sourcing teams all need to sign off before nomination.
Recommended checklist
- Confirm kit scope, intended use environment, and annual demand band, such as under 1,000 sets, 1,000 to 10,000 sets, or higher-volume programs.
- Request sample records that show how instruments, accessories, trays, and labels are controlled as one finished kit.
- Review documentation responsiveness, including material certificates, traceability references, and revision records.
- Evaluate lead-time logic for first order, repeat order, and urgent replenishment scenarios.
- Clarify change control: who approves substitutions, when notice is required, and how changes are documented.
- Check whether the supplier can support packaging, labeling, and configuration needs across your target market footprint.
For procurement leaders who need stronger technical confidence, independent benchmarking can add value by separating sales positioning from measurable process evidence. That is especially useful when comparing suppliers that appear similar on paper but differ in documentation rigor, consistency risk, or long-term support capability.
Why work with a technical benchmarking partner before committing
At VitalSync Metrics, we focus on the question procurement teams actually face: is this supplier suitable for the intended healthcare supply scenario, and what evidence supports that conclusion? For surgical instrument kits OEM assessments, that may include reviewing manufacturing parameters, documentation structure, material-related considerations, and risk indicators that affect sourcing confidence over time.
Because healthcare procurement is moving toward tighter compliance expectations and more data-driven vendor qualification, buyers increasingly need clearer ways to compare technical integrity, not just commercial offers. An external benchmarking perspective can help identify whether a supplier is best suited for hospital replenishment programs, distributor scale-up, or development-stage kit projects. That reduces the chance of selecting a partner whose strengths do not match the actual use case.
If you are currently reviewing surgical instrument kits OEM options, we can help you narrow the shortlist with scenario-based criteria. Contact us to discuss parameter confirmation, kit configuration review, supplier comparison logic, documentation expectations, sample support, target lead times, and quotation alignment. Whether you are qualifying a new OEM, comparing private label candidates, or validating a specialized kit program, the next step should be based on evidence, not assumption.
Recommended News
- 2026.04.29Healthcare Analytics Metrics That Support Smarter Budget CallsLydia Vancini (Regulatory Compliance Lead)
- 2026.04.29Mobility Assist Selection Mistakes That Limit Long-Term UseSarah Jenkins (Laboratory Infrastructure Consultant)
- 2026.04.29Endoscope Image Resolution Benchmark for Vendor ComparisonDr. Alistair Thorne (Senior Biomedical Engineer)
The VitalSync Intelligence Brief
Receive daily deep-dives into MedTech innovations and regulatory shifts.
